Here's something most fertility clinics won't tell you: your egg quality isn't fixed. Yes, age matters — I'll get into exactly how much in a moment — but it's not the only thing that matters. And the idea that you're powerless to influence the health of your eggs? That's outdated, incomplete, and in my experience, genuinely harmful to women who deserve better information.
I know this because I lived it. At 32, my AMH came back at around 3 pmol/L — a number that should have been above 20 for my age. Clinics told me egg freezing was my only realistic option. One doctor actually said that nutrition couldn't make any difference. I refused to accept that, built my own evidence-based protocol, and two years later my AMH had more than doubled to 6.43. I'm now mum to a healthy baby boy called Bowie, conceived naturally.
This article is everything I've learned — from my own journey, from my master's research in nutritional science, and from working with hundreds of clients in my clinic. Whether you're trying to conceive naturally, preparing for IVF, or you've been told your egg quality is declining with age, there's a lot more within your control than you think.
What Egg Quality Actually Means
When fertility specialists talk about egg quality, they're really talking about two things: whether your egg has the correct number of chromosomes (euploidy), and whether it has enough cellular energy to divide properly after fertilisation.
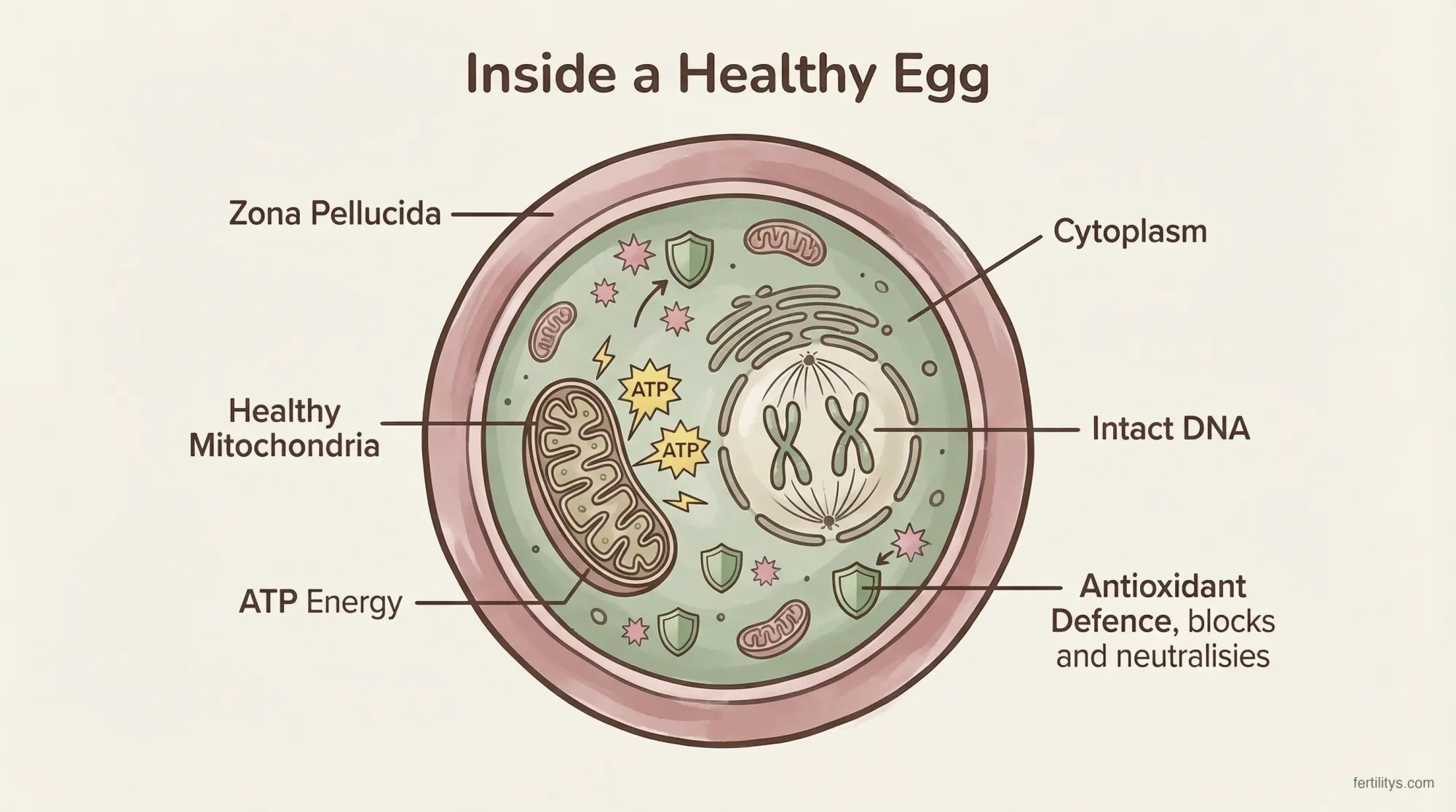
Every egg in your ovaries is a single cell — but it's not a simple one. Each contains roughly 100,000 to 600,000 mitochondria, the tiny energy generators inside every cell. That's more mitochondria than almost any other cell type in your body. And that matters enormously, because the process of an egg maturing, being fertilised, and dividing into an embryo is incredibly energy-intensive.
When we talk about "poor egg quality," what's usually happening at a cellular level is one or both of these:
- Mitochondrial dysfunction — the egg doesn't produce enough ATP (cellular energy) for proper chromosome separation during division
- Oxidative damage — accumulated free radical damage to the egg's DNA, membranes, and mitochondria
The result? Higher rates of chromosomal abnormalities (aneuploidy), failed fertilisation, poor embryo development, or early miscarriage. A study by Cecchino et al. (2018) in Fertility and Sterility found that chromosomal abnormalities account for roughly 60-70% of early pregnancy losses.
Here's the part that gives me hope: both mitochondrial function and oxidative stress are modifiable. Not perfectly, not for every woman in every situation — but meaningfully, measurably, and often dramatically.
How Age Affects Egg Quality
I won't pretend age doesn't matter — it does, and being honest about that is part of respecting your intelligence. But the relationship between egg quality and age is more nuanced than most clinics communicate.
You're born with all the eggs you'll ever have — roughly 1-2 million at birth, declining to about 300,000-400,000 by puberty. By your late 30s, you're down to around 25,000. But egg quantity and egg quality are different conversations.
Quality decline accelerates after 35 and becomes steeper after 38. By 40, roughly 60-80% of eggs may be chromosomally abnormal (aneuploid), compared with about 20-30% in your early 30s. By 43, that figure can exceed 90% (Franasiak et al., 2014, Fertility and Sterility).
The primary driver? Mitochondrial ageing. As Li et al. (2024) documented in Frontiers in Endocrinology, maternal age significantly decreases both the number and quality of mitochondria in oocytes. Older eggs produce less ATP, accumulate more reactive oxygen species (ROS), and have higher rates of DNA damage.
But — and this is the part I wish someone had told me at 32 — these processes are influenced by far more than just your birth date. Two women of the same age can have wildly different egg quality depending on their nutrition, supplementation, toxic load, stress levels, and lifestyle. That's the window of opportunity we're working with.
The 90-Day Window
Eggs take approximately 90 days to mature from a dormant primordial follicle to an ovulation-ready oocyte. During those three months, the developing egg is actively building mitochondria, accumulating nutrients, and responding to your internal environment. This is why I tell every client: what you do in the 3 months before conception — or before an IVF cycle — genuinely shapes the quality of the egg you ovulate.
And honestly? Three months is a minimum. I started my own protocol more than a year before conceiving, and I believe that longer preparation window was part of why it worked. The research on preconception nutrition supports this — changes to diet and lifestyle need time to cascade through your biology.
🕐 Start Earlier Than You Think
Most fertility guidance focuses on a 3-month preparation window. I believe that's a minimum, not a target. I started my own protocol more than a year before conceiving, and the research on preconception nutrition supports longer preparation periods. If you're planning to try for a baby — or thinking about it — start optimising now. The earlier you begin, the more time your eggs have to benefit.
Supplements That Support Egg Quality

I'm a nutritionist with a food-first philosophy. But when it comes to egg quality specifically, there are a handful of supplements with genuinely strong evidence — and a few that were central to my own protocol. Here's what the research actually says.
CoQ10 (Coenzyme Q10)
If I could only recommend one supplement for egg quality, it would be CoQ10. It sits right at the centre of the mitochondrial energy story.
CoQ10 is a coenzyme that lives inside your mitochondria and is essential for producing ATP. Your body makes it naturally, but production declines with age — exactly when your eggs need it most. The landmark animal study by Ben-Meir et al. (2015) in Aging Cell showed that CoQ10 supplementation restored oocyte mitochondrial function and reversed age-related fertility decline in mice.
In humans, the evidence has become increasingly strong. A 2024 systematic review and meta-analysis by Xu et al., published in Annals of Medicine, analysed data from multiple randomised controlled trials of women with diminished ovarian reserve undergoing IVF. The results were striking: CoQ10 pretreatment was associated with an 84% increase in clinical pregnancy rates (OR 1.84), significantly more oocytes retrieved, more high-quality embryos, and a 40% reduction in cycle cancellation rates.
I took 200mg of ubiquinol (the active, reduced form of CoQ10) daily for over two years. Most clinical trials use 200-600mg per day, starting at least 2-3 months before conception or an IVF cycle. Ubiquinol is absorbed better than ubiquinone, especially over age 30 when your body's ability to convert between the two starts to slow.
Vitamin D
Vitamin D deficiency is staggeringly common — the UK's National Diet and Nutrition Survey found that around 1 in 5 adults in the UK have serum levels below 25 nmol/L. And it turns out this matters enormously for egg quality.
Baldini et al. (2024) published a study in Archives of Gynecology and Obstetrics showing that vitamin D supplementation improved embryo quality in IVF patients regardless of their baseline vitamin D status. An earlier meta-analysis by Chu et al. (2018) in Human Reproduction found that women with sufficient vitamin D levels had significantly higher clinical pregnancy and live birth rates from IVF.
The mechanism appears to involve vitamin D receptors on granulosa cells (the cells surrounding and nourishing your developing egg). Adequate vitamin D supports anti-Müllerian hormone production, follicular development, and progesterone synthesis. I take 10mcg (400 IU) daily — the UK recommended dose — year-round. Some fertility specialists recommend higher doses of 1,000-2,000 IU, particularly if blood tests show deficiency.
DHEA (Dehydroepiandrosterone)
DHEA is a hormone your adrenal glands produce, and it's a precursor to both oestrogen and testosterone. Levels decline with age, and supplementation has become common in fertility clinics — particularly for women with diminished ovarian reserve.
A 2024 network meta-analysis combining 38 studies (published across multiple databases) found that DHEA supplementation improved the number of eggs retrieved and clinical pregnancy rates in women with poor ovarian response. Schwarze et al. (2018) had previously shown similar results specifically for IVF/ICSI outcomes.
Important: DHEA is a hormone, not a simple vitamin. It should only be taken under medical supervision, typically at 25mg three times daily for 6-12 weeks before an IVF cycle. It's not appropriate for everyone — women with PCOS, for example, may already have elevated androgen levels. I mention it here because it's part of the conversation, but please discuss it with your fertility specialist before starting.
Omega-3 Fatty Acids
Omega-3s — specifically DHA and EPA from fish oil — support egg quality through their anti-inflammatory properties and their role in cell membrane integrity. Your eggs need healthy, flexible cell membranes for proper division.
Hammiche et al. (2011) found that higher omega-3 intake was associated with better embryo morphology, while Chiu et al. (2018) in Human Reproduction linked higher omega-3 blood levels to improved oocyte and embryo quality in women undergoing IVF. I take a daily fish oil supplement and eat oily fish (salmon, mackerel, sardines) at least twice a week.
Melatonin
Most people know melatonin as a sleep hormone, but it's also one of the most powerful antioxidants in your body — and it concentrates heavily in ovarian follicular fluid, right where your developing eggs sit.
Tamura et al. (2008) demonstrated that melatonin protects oocytes from free radical damage and improves fertilisation rates. A 2024 meta-analysis by Shang et al. confirmed that combining melatonin with CoQ10 increased the number of oocytes collected during IVF. The typical dose used in fertility research is 3mg taken at bedtime, and it has the added benefit of improving sleep quality — something that directly supports your fertility anyway.
Folate (as Methylfolate)
You probably know folate (vitamin B9) as a pregnancy supplement for preventing neural tube defects. But it's also involved in DNA synthesis and repair within your developing eggs. Roughly 40-60% of the population carries the MTHFR gene variant that reduces the ability to convert folic acid into its active form, methylfolate (5-MTHF). I recommend methylfolate over standard folic acid — at least 400mcg daily, starting well before conception.
What About NAC, Alpha-Lipoic Acid, and Resveratrol?
These antioxidants show promise in animal and preliminary human studies. N-acetyl cysteine (NAC) boosts glutathione — your body's master antioxidant. Alpha-lipoic acid (ALA) supports mitochondrial energy production. Resveratrol has shown anti-ageing effects on oocytes in animal models. But the human clinical evidence is still emerging, and I don't include them in my core recommendations yet. Worth discussing with your practitioner if you want to explore a more comprehensive protocol.
Diet and Egg Quality
Supplements support your eggs, but your diet is the foundation. And the evidence here is clearer than many people realise.
Karayiannis et al. (2018) published a landmark study in Human Reproduction showing that non-obese women who closely followed a Mediterranean diet had significantly higher IVF success rates — with a 2.7 times greater likelihood of achieving clinical pregnancy and live birth. The Mediterranean pattern — rich in vegetables, fruits, whole grains, legumes, fish, and olive oil — provides the broad spectrum of antioxidants, healthy fats, and micronutrients that developing eggs need.
When I got my low AMH diagnosis, one of the first things I overhauled was my diet. I shifted to a Mediterranean eating pattern, prioritised organic produce, increased my vegetable and berry intake dramatically, and eliminated refined sugar. I focused on:
- Antioxidant-rich berries — blueberries, raspberries, strawberries (organic — see the Dirty Dozen below)
- Leafy greens — spinach, kale, broccoli for folate and iron
- Healthy fats — avocado, olive oil, nuts, seeds, oily fish
- Quality protein — eggs, wild-caught fish, legumes, small amounts of organic poultry
- Complex carbohydrates — sweet potatoes, quinoa, oats for steady blood sugar
Blood sugar stability matters more for egg quality than most people think. Jakubowicz et al. (2013) showed that insulin resistance directly impairs ovarian function, and even women without PCOS can have subclinical insulin issues that affect egg development. I cut refined sugars completely and made sure every meal included protein, fat, and fibre to slow glucose absorption.
🍎 Go Organic With the Dirty Dozen
These twelve fruits and vegetables carry the heaviest pesticide loads. I tell all my clients: if you can only afford to go organic on some things, make it these. The rest you can buy conventional and wash well.
The list: Strawberries, spinach, kale/collard/mustard greens, peaches, pears, nectarines, apples, grapes, bell & hot peppers, cherries, blueberries, green beans (EWG, 2025).
Baudry et al. (2018) found that women who ate organic food most frequently had a 24% lower risk of infertility compared with those who rarely ate organic. The mechanism? Lower pesticide exposure reduces the oxidative burden on your eggs. This is particularly relevant for the heavily sprayed produce on the Dirty Dozen list — and it's why I went fully organic on fruits and vegetables during my fertility preparation.
Lifestyle Changes That Genuinely Matter
Exercise — Less May Be More

This one surprised me. I used to do high-intensity interval training five or six times a week and thought I was the picture of health. But the research tells a more complex story.
Moderate exercise supports fertility — walking, swimming, yoga, light cycling. But excessive intense exercise can raise cortisol, disrupt hormonal signalling, and potentially impair egg development. Wise et al. (2012) found that vigorous physical activity was associated with reduced fecundability, while moderate activity had a positive or neutral effect.
I gave up HIIT completely and switched to walking, gentle yoga, and fertility-specific acupuncture. One of my clients was doing intense CrossFit five days a week and had been trying for over a year — we scaled right back to walking and restorative yoga, and she conceived within four months. I can't prove the exercise change was the deciding factor, but the pattern I see in my practice is consistent: gentler movement, better outcomes.
Sleep
Your eggs repair and develop during sleep. Melatonin — the antioxidant that protects your oocytes — is produced primarily during darkness, with peak production between 2am and 4am. A 2024 study in PLoS ONE (Yi et al.) demonstrated that total sleep deprivation caused oxidative stress and mitochondrial dysfunction in oocytes, directly reducing egg quality in animal models.
I made eight hours a non-negotiable. No screens after 9pm, blackout curtains, cool bedroom, consistent sleep and wake times. It sounds basic, but your biology rewards consistency.
Stress Management
Chronic stress elevates cortisol, which can suppress GnRH (the hormone that triggers your entire reproductive cascade) and divert resources away from reproduction. I'm not going to tell you to "just relax" — that advice is unhelpful and dismissive. But actively managing your stress response through specific practices makes a measurable difference.
I used fertility acupuncture (weekly during my preparation phase), daily meditation, and yoga. The evidence on acupuncture is mixed but promising — several systematic reviews suggest it may improve blood flow to the ovaries and reduce stress hormones. At minimum, it gave me a regular hour of stillness in a period that was emotionally turbulent.
Toxin Reduction
Environmental toxins — particularly endocrine disruptors like BPA, phthalates, and certain pesticides — can directly damage egg quality by interfering with hormone signalling and increasing oxidative stress. Mínguez-Alarcón et al. (2019) linked higher urinary BPA levels to lower oocyte yield and poorer embryo quality in IVF patients.
My toxin audit was thorough. I removed plastic food containers (switched to glass), stopped using synthetic perfumes, swapped to natural cleaning products, and — non-negotiably — cut out alcohol completely. I also went fully organic on produce. It felt like a lot of change at once, but once the new habits were in place, it was straightforward.
And I'll say this directly: if you're using recreational drugs of any kind — cannabis, cocaine, MDMA, anything — and you're trying to conceive, stop. The evidence on their effects on egg and sperm quality is unambiguous, and this is one area where there's no debate.
How to Improve Egg Quality for IVF
Everything above applies whether you're conceiving naturally or through IVF — but there are a few IVF-specific considerations worth highlighting.
The most impactful window is the 2-3 months before your stimulation cycle begins. This is when your eggs are actively maturing and most responsive to nutritional and lifestyle optimisation. Start your supplement protocol early — CoQ10, vitamin D, omega-3s, and methylfolate as a minimum. Add melatonin (3mg at bedtime) from 6-8 weeks before egg retrieval if your specialist approves.
The 2024 meta-analysis by Xu et al. specifically studied women with diminished ovarian reserve undergoing IVF/ICSI. CoQ10 pretreatment led to more oocytes retrieved, more high-quality embryos, and fewer cancelled cycles. For women with low AMH or a previous poor response, this data is particularly encouraging.
Work with your clinic, not against it. Show them the research. Most reproductive endocrinologists are now open to supplementation protocols alongside standard treatment — the evidence base has grown substantially in recent years, and attitudes are shifting.
Can You Improve Egg Quality After 40?
Yes — but with realistic expectations. After 40, the proportion of chromosomally normal eggs is smaller, and no supplement can undo decades of mitochondrial ageing overnight. What you can do is optimise the eggs you have.
The strategies are the same: CoQ10 (some specialists recommend higher doses of 400-600mg for women over 40), vitamin D, omega-3s, Mediterranean diet, stress reduction, gentle exercise, toxin avoidance. DHEA may be particularly relevant here — discuss with your fertility specialist, as the evidence for improved ovarian response in older women is among the stronger findings in the DHEA literature.
What changes is the urgency. If you're 40 or over and trying to conceive, you don't have the luxury of a leisurely 12-month preparation window. Start immediately, implement everything in parallel, and consider working with both a fertility nutritionist and a reproductive endocrinologist simultaneously. Every month counts.
I want to be clear: I'm not promising miracles. Some women over 40 will conceive naturally with optimised egg quality. Others will need IVF, donor eggs, or will face outcomes that no amount of preparation could have changed. What I am saying is that doing nothing because "it's just age" is leaving opportunities on the table. The research supports taking action, and I've seen it make a difference in my clinic repeatedly.
What Doesn't Work (and What to Watch Out For)
Not everything marketed as an egg quality solution has evidence behind it. A few things worth knowing:
- "Fertility cleanses" — no evidence they improve egg quality. Your liver and kidneys handle detoxification. Eat clean, reduce toxin exposure, and let your body do its job.
- Extreme calorie restriction — actively harmful. Your eggs need energy to develop. Very low-calorie diets can disrupt ovulation entirely.
- Mega-dose antioxidants without guidance — more is not always better. Excess vitamin E, for example, can become pro-oxidant at high doses. Stick to evidence-based dosing.
- Products claiming to "reverse ovarian age" — be sceptical. You can improve the quality of the eggs you have. You cannot increase the total number of eggs in your ovaries or reverse true ovarian ageing.
If a product sounds too good to be true, it almost certainly is. The real approach isn't glamorous — it's consistent, evidence-based, and requires patience.
The Bottom Line
Egg quality isn't a fixed sentence handed down by your age. It's a dynamic biological state influenced by your mitochondrial health, your oxidative stress burden, your nutrition, your lifestyle, and — yes — your age. You can't control when you were born. But you can control what you eat, which supplements you take, how you move, how you sleep, and what you expose your body to.
I'm living proof of that. My AMH went from 3 to 6.43. Clinics told me a natural pregnancy was unlikely. Bowie is sleeping in the next room as I write this.
Start early — ideally a year before you want to conceive, not just the commonly cited three months. Build your protocol around CoQ10, vitamin D, omega-3s, and methylfolate. Eat a Mediterranean diet. Move gently. Sleep properly. Reduce your toxic load. And if you're preparing for IVF, bring this evidence to your clinic.
Your eggs are listening to your body. Give them the best environment you can.
FAQ
▸How long does it take to improve egg quality?
Eggs take approximately 90 days to mature from dormant follicle to ovulation-ready oocyte. Most supplements and lifestyle changes need at least 2-3 months to influence egg quality meaningfully. I recommend starting at least 3 months before trying to conceive — ideally 6-12 months for a more comprehensive approach.
▸Can you test egg quality without IVF?
There's no direct test for egg quality outside of IVF (where embryo grading gives an indication). AMH and antral follicle count measure egg quantity, not quality. Age remains the strongest predictor. However, some specialists use a combination of AMH, FSH, and antral follicle count alongside age to estimate likely quality.
▸What is the best supplement for egg quality?
CoQ10 (coenzyme Q10) has the strongest evidence base. A 2024 meta-analysis found it increased clinical pregnancy rates by 84% in women with diminished ovarian reserve. Take 200-600mg daily in the ubiquinol form for better absorption. Vitamin D, omega-3s, and methylfolate are also well-supported.
▸Does egg quality decline after 35?
Egg quality does decline more noticeably after 35, with a steeper decline after 38. By 40, roughly 60-80% of eggs may be chromosomally abnormal. However, this is an average — individual variation is significant, and lifestyle factors can influence where you fall within that range.
▸Can improving egg quality help with recurrent miscarriage?
Chromosomal abnormalities (often linked to egg quality) are the leading cause of early miscarriage, accounting for 60-70% of first-trimester losses. Supporting egg quality through supplementation and lifestyle changes may reduce the risk of aneuploid eggs, though recurrent miscarriage can have other causes that need medical investigation.
▸Is it too late to improve egg quality at 42?
It's not too late, but the window is narrower. At 42, a higher proportion of eggs will be chromosomally abnormal, and you'll have fewer remaining. Optimising the eggs you do have through CoQ10, diet, and lifestyle changes is still worthwhile — particularly if you're preparing for IVF. Work with a reproductive endocrinologist alongside nutritional support for the best outcomes.
▸Does diet really affect egg quality?
Yes. Karayiannis et al. (2018) found that women following a Mediterranean diet were 2.7 times more likely to achieve clinical pregnancy and live birth through IVF. Diet affects egg quality through antioxidant protection, anti-inflammatory pathways, blood sugar regulation, and providing the micronutrients eggs need during their 90-day maturation period.
▸How long does it take to improve egg quality?
The egg maturation process takes approximately 90 days (3 months), so most fertility specialists recommend starting supplements and lifestyle changes at least 3 months before trying to conceive or starting IVF.
▸What supplements improve egg quality?
The strongest evidence supports CoQ10 (200-600mg), vitamin D (if deficient), omega-3 fatty acids, folate/methylfolate, and antioxidants like vitamin E and alpha-lipoic acid. DHEA is sometimes recommended under medical supervision for diminished ovarian reserve.
▸Does age affect egg quality?
Yes. Egg quality naturally declines with age, primarily due to increased chromosomal abnormalities. This is the main reason fertility decreases after 35. While you can't stop this process, good nutrition and lifestyle choices may slow the rate of decline.
You might also find helpful:
References
- Ben-Meir A, Burstein E, Borrego-Alvarez A, et al. Coenzyme Q10 restores oocyte mitochondrial function and fertility during reproductive aging. Aging Cell. 2015;14(5):887-895. doi:10.1111/acel.12368
- Xu Y, Nisenblat V, Lu C, et al. Clinical evidence of coenzyme Q10 pretreatment for women with diminished ovarian reserve undergoing IVF/ICSI: a systematic review and meta-analysis. Annals of Medicine. 2024;56(1):2389469. doi:10.1080/07853890.2024.2389469
- Franasiak JM, Forman EJ, Hong KH, et al. The nature of aneuploidy with increasing age of the female partner. Fertility and Sterility. 2014;101(3):656-663. doi:10.1016/j.fertnstert.2013.11.024
- Li J, Gao Y, Guan L, et al. Mechanisms of mitochondrial dysfunction in ovarian aging and potential interventions. Frontiers in Endocrinology. 2024;15:1361289. doi:10.3389/fendo.2024.1361289
- Baldini GM, Russo M, Proietti S, et al. Supplementation with vitamin D improves the embryo quality in IVF programs, independently of patients' basal vitamin D status. Archives of Gynecology and Obstetrics. 2024;310:1481-1490. doi:10.1007/s00404-024-07473-7
- Chu J, Gallos I, Tobias A, et al. Vitamin D and assisted reproductive treatment outcome: a systematic review and meta-analysis. Human Reproduction. 2018;33(1):65-80. doi:10.1093/humrep/dex326
- Tamura H, Takasaki A, Miwa I, et al. Oxidative stress impairs oocyte quality and melatonin protects oocytes from free radical damage and improves fertilization rate. Journal of Pineal Research. 2008;44(3):280-287. doi:10.1111/j.1600-079X.2007.00524.x
- Karayiannis D, Kontogianni MD, Mendorou C, et al. Adherence to the Mediterranean diet and IVF success rate among non-obese women attempting fertility. Human Reproduction. 2018;33(3):494-502. doi:10.1093/humrep/dey003
- Jakubowicz D, Barnea M, Wainstein J, et al. Effects of caloric intake timing on insulin resistance and hyperandrogenism in lean women with polycystic ovary syndrome. Clinical Science. 2013;125(9):423-432. doi:10.1042/CS20130071
- Baudry J, Assmann KE, Touvier M, et al. Association of frequency of organic food consumption with cancer risk. JAMA Internal Medicine. 2018;178(12):1597-1606. doi:10.1001/jamainternmed.2018.4357
- Wise LA, Rothman KJ, Mikkelsen EM, et al. A prospective cohort study of physical activity and time to pregnancy. Fertility and Sterility. 2012;97(5):1136-1142. doi:10.1016/j.fertnstert.2012.02.025
- Yi ZY, Liang QX, Zhou Q, et al. Maternal total sleep deprivation causes oxidative stress and mitochondrial dysfunction in oocytes. PLoS ONE. 2024;19(10):e0306152. doi:10.1371/journal.pone.0306152
- Mínguez-Alarcón L, Gaskins AJ, Chiu YH, et al. Urinary bisphenol A concentrations and association with in vitro fertilization outcomes among women from a fertility clinic. Human Reproduction. 2015;30(9):2120-2128. doi:10.1093/humrep/dev183
- Chiu YH, Karmon AE, Gaskins AJ, et al. Serum omega-3 fatty acids and treatment outcomes among women undergoing assisted reproduction. Human Reproduction. 2018;33(1):156-165. doi:10.1093/humrep/dex335
- Cecchino GN, Seli E, Alves da Motta EL, García-Velasco JA. The role of mitochondrial activity in female fertility and assisted reproductive technologies. Journal of Assisted Reproduction and Genetics. 2018;35(9):1573-1588. doi:10.1007/s10815-018-1266-z
Medical Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always consult your healthcare provider or fertility specialist before starting any supplement protocol or making significant dietary changes, particularly if you are undergoing fertility treatment. Individual results vary, and what worked for me may not be appropriate for your specific situation.
All my Free Resources. No spam. Unsubscribe anytime.















