Key Takeaways
- Stress delays your period by suppressing GnRH pulses in the hypothalamus, which delays or prevents ovulation
- Cortisol — your body's stress hormone — directly interferes with LH and FSH, the hormones that drive your menstrual cycle
- A 2024 systematic review confirmed that elevated psychological stress is consistently linked to menstrual irregularity
- Both acute stress (a bereavement, job loss) and chronic stress (ongoing work pressure, fertility anxiety) can affect your cycle
- A late period from stress is not dangerous — but if your period is late by more than three cycles, see your GP
You're staring at a calendar, counting days, and your period still hasn't arrived. You're not pregnant — you've tested. So what's going on?
If you've been under more pressure than usual lately, you probably already suspect the answer. And you're right to. Stress is one of the most common — and most underestimated — reasons for a late period.
I see this constantly with my clients. A woman who's been tracking her cycle like clockwork suddenly finds herself five, eight, twelve days late. Nothing else has changed — except her stress levels went through the roof. Maybe she's in the middle of fertility treatment. Maybe work imploded. Maybe she's grieving.
The connection between your brain and your reproductive system is far more direct than most people realise. And understanding exactly how stress affects your cycle can actually help you do something about it.
How Stress Actually Delays Your Period
Your menstrual cycle isn't controlled by your ovaries alone — it starts in your brain. Specifically, in a tiny region called the hypothalamus, which acts as the control centre for your reproductive hormones.
Here's the chain of events in a normal cycle: your hypothalamus releases GnRH (gonadotropin-releasing hormone) in precise pulses. These pulses tell your pituitary gland to release FSH and LH — the hormones that stimulate your ovaries to develop a follicle and eventually trigger ovulation. After ovulation, progesterone rises, and about 14 days later, your period arrives.
When you're stressed, your body activates what's called the HPA axis — the hypothalamic-pituitary-adrenal axis. This is your fight-or-flight system. It floods your body with cortisol and CRH (corticotropin-releasing hormone), and here's where the problem starts: CRH directly suppresses those GnRH pulses. No GnRH pulses, no LH surge. No LH surge, no ovulation. No ovulation, no period — or at least, a significantly delayed one.
Berga and Loucks (2005) demonstrated that women with stress-related amenorrhoea had measurably higher cortisol levels and suppressed LH pulsatility compared to women with regular cycles. The mechanism is clear and well-documented — your brain is literally telling your reproductive system to stand down because it perceives a threat.
"Your body can't tell the difference between being chased by a tiger and being crushed by a work deadline," is how I explain it to clients. From your hypothalamus's perspective, stress is stress. And when survival feels threatened, reproduction gets deprioritised.

What Counts as "Enough" Stress to Affect Your Cycle?
This is the question I get asked most — and the honest answer is that it varies enormously from person to person. There's no stress threshold that universally triggers a late period. Your genetics, baseline cortisol levels, sleep quality, nutrition, and even your gut microbiome all influence how resilient your cycle is. Your individual level of stress tolerance is unique — what disrupts one woman's cycle won't touch another's.
That said, research gives us some patterns. A 2024 systematic review by Kolhe et al., published in Neuroscience & Biobehavioral Reviews, analysed decades of studies on psychological stress and menstrual irregularity. Their finding was unequivocal: elevated stress is consistently associated with irregular menstruation, including delayed periods, shorter cycles, and heavier or lighter bleeding.
The types of stress most commonly linked to cycle disruption include:
- Major life events — bereavement, divorce, moving house, job loss, financial crisis
- Chronic workplace stress — particularly jobs with high demand and low control
- Fertility-related anxiety — the cruel irony that stressing about getting pregnant can delay the very cycle you're tracking
- Relationship stress — conflict, loneliness, or emotional instability
- Academic pressure — studies of university students consistently show higher rates of menstrual irregularity during exam periods
- Sleep disruption — which both causes and amplifies cortisol dysregulation
I worked with a client in her late twenties who'd had textbook 28-day cycles her entire adult life. She started a new job, went through a breakup the same month, and her period vanished for seven weeks. No pregnancy. No underlying condition. Just her nervous system hitting the brakes on ovulation until things calmed down.
How Long Can Stress Delay Your Period?
A few days is common. A week or two isn't unusual. In extreme cases — severe or prolonged stress — your period can disappear entirely for months. Doctors call this functional hypothalamic amenorrhoea (FHA), and it's the most common cause of secondary amenorrhoea in women of reproductive age, according to a 2023 review in Mayo Clinic Proceedings.
The key word is "functional" — meaning there's nothing structurally wrong with your reproductive organs. Your system is working exactly as designed. It's just responding to a signal from your brain that says "now is not a safe time to reproduce."
What matters most isn't the duration of the delay but whether your cycle returns to normal once the stressor resolves. For most women, it does. Your period may take one to three cycles to return after the stress reduces — though it might be lighter or heavier than usual for a cycle or two while your hormones recalibrate.
If your period has been absent for three months or more, that's worth investigating with your GP. Not because it's dangerous in itself, but because prolonged low oestrogen (which accompanies prolonged anovulation) can affect your bone density and cardiovascular health over time.
Stress, Late Period, or Pregnancy?
Let's address the question that's probably really on your mind: how do you know if your late period is from stress or because you're pregnant?
The short answer: take a test. A home pregnancy test is reliable from the day your period is due. If it's negative and you're more than a week late, test again three days later with first-morning urine. Two negative tests a week apart, and you can be confident it's not pregnancy.
The symptoms don't help much for distinguishing between the two — stress and early pregnancy share an almost identical symptom profile: breast tenderness, fatigue, nausea, mood swings, bloating. That's because both involve progesterone fluctuations, and progesterone doesn't care about the cause — it produces the same physical effects regardless.
If you're actively trying to conceive, this overlap can be emotionally brutal. You're symptom-spotting, hoping every twinge is implantation, and the stress of the two-week wait itself is enough to push your period back further. I've been there myself during my fertility journey — those extra days of waiting felt endless.
The Fertility-Stress Cycle (And How to Break It)
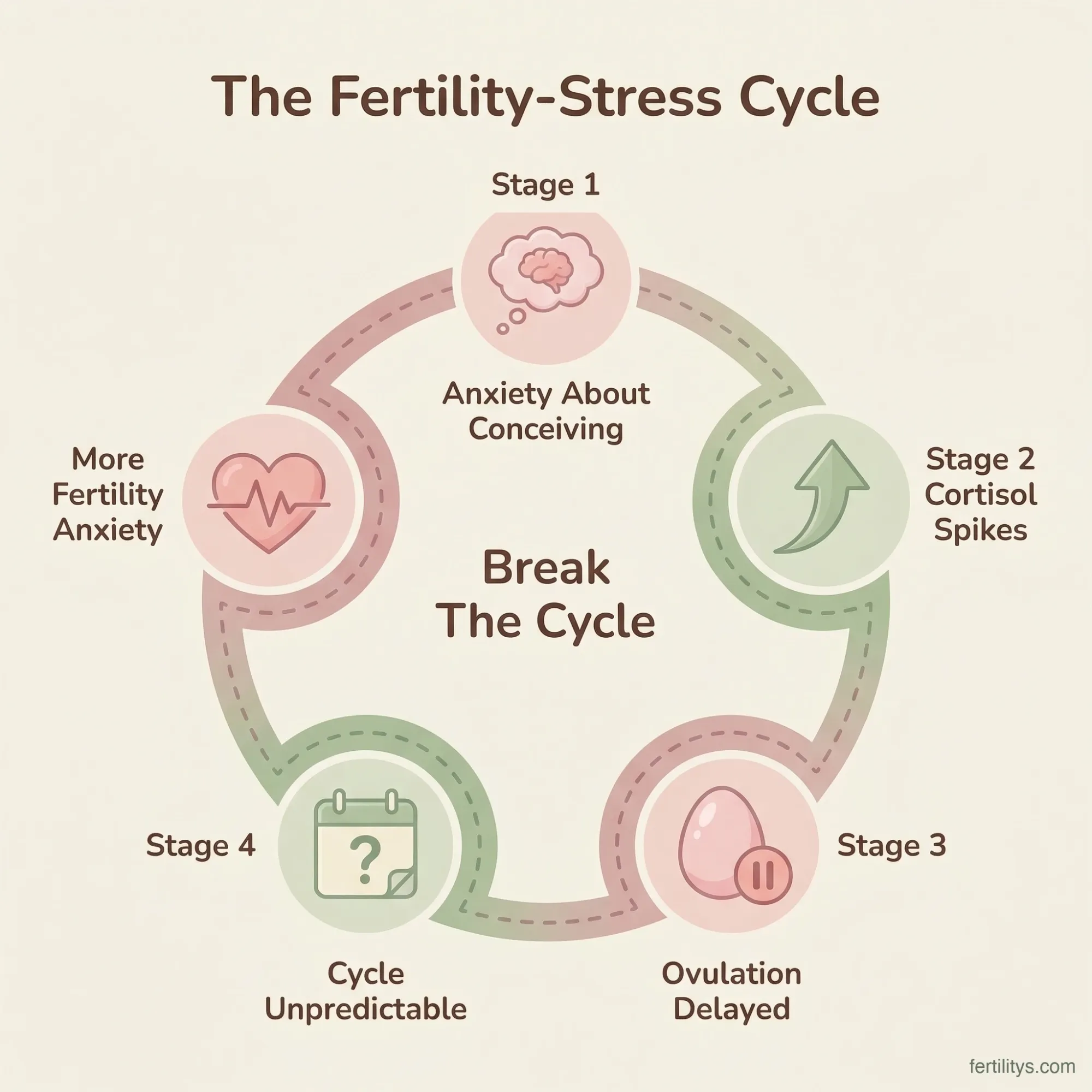
This is the part that frustrates me most as a nutritionist, because it's a genuine catch-22. Stress can delay ovulation. Delayed ovulation means a longer cycle. A longer cycle means more time worrying about whether you've ovulated at all. More worry means more cortisol. More cortisol means further suppression of GnRH. And round and round it goes.
If you're trying to conceive, this cycle can feel impossible to escape. Everyone tells you to "just relax" — which, as anyone who's been through fertility struggles knows, is about as helpful as being told to "just sleep" when you have insomnia.
But there are evidence-based strategies that genuinely help lower cortisol and support your cycle. Not because relaxation is a magic fertility cure, but because reducing HPA axis activation gives your hypothalamus the space to restore normal GnRH pulsatility.
Blood sugar stability. Cortisol spikes when blood sugar crashes. Eating regular meals with protein, fat, and complex carbohydrates at each meal helps keep cortisol steady throughout the day. This is one of the first things I address with clients — often before we even talk about supplements.
Gentle movement over intense exercise. High-intensity training elevates cortisol further. Walking, yoga, swimming, and Pilates support your nervous system without adding physiological stress. I stopped HIIT completely during my own fertility journey and switched to yoga and walking — it made a noticeable difference to my cycle regularity.
Sleep hygiene. Cortisol follows a circadian rhythm — it should peak in the morning and drop at night. Poor sleep disrupts this pattern. Aim for 7-9 hours, keep your bedroom cool and dark, and try to maintain consistent wake and sleep times even on weekends.
Targeted nutrition. Magnesium glycinate (300-400mg before bed) supports HPA axis regulation and sleep quality. Omega-3 fatty acids (particularly EPA) have anti-inflammatory effects that help modulate cortisol. Vitamin B6 supports progesterone production. These aren't miracle cures — they're foundational support for a nervous system that's running too hot.
Stress-specific practices. Yoga Nidra, progressive muscle relaxation, and breathwork (particularly extended exhale patterns like 4-7-8 breathing) directly activate the parasympathetic nervous system. A 2015 study by Youngs et al. showed that an 8-week mindfulness programme significantly reduced perceived stress and improved menstrual regularity in women with stress-related cycle disruption.
When to See Your Doctor
A one-off late period during a stressful month is normal. But there are situations where you should get checked:
- Your period has been absent for three months or more (the clinical definition of amenorrhoea)
- You're experiencing other symptoms — significant weight changes, hair loss, excessive hair growth, severe acne, or milky discharge from your breasts
- You've had consistently irregular cycles (varying by more than 7-9 days month to month) for six months or longer
- You're trying to conceive and your cycles are unpredictable — this directly affects your ability to time intercourse around ovulation
- You suspect you might have polycystic ovary syndrome (PCOS) or a thyroid condition — both cause irregular periods and are often mistaken for stress-related delays
It's also worth noting that recently stopping birth control can cause similar cycle disruption — if you've come off hormonal contraception in the last few months, that could be a contributing factor alongside stress. Your GP will likely run blood tests for FSH, LH, oestradiol, prolactin, thyroid function, and possibly testosterone and DHEAS. These help distinguish between stress-related cycle disruption and other conditions like PCOS, thyroid disease, or premature ovarian insufficiency.
The Bottom Line
Your period is a vital sign — a monthly report card on your overall health, not just your reproductive system. When stress delays it, that's your body telling you something needs to change. Not in a panicky way, but in a "please pay attention to this" way.
The reassuring news is that stress-related period delays are almost always temporary and completely reversible. Your cycle wants to be regular. Given the right conditions — adequate nutrition, manageable stress levels, enough sleep, gentle movement — it will find its rhythm again.
And if you're trying to conceive and stress is disrupting your cycle, please don't add "I'm stressed about being stressed" to your worry list. Focus on the practical interventions — blood sugar, sleep, movement, nutrition — and give your body the support it needs. The hormonal cascade that controls your cycle is remarkably responsive to these changes.
▸Can stress make your period late?
Yes. Stress raises cortisol, which suppresses the GnRH pulses your brain needs to trigger ovulation. When ovulation is delayed, your entire cycle shifts later. This can delay your period by a few days to several weeks, depending on the severity and duration of the stress.
▸How many days can stress delay your period?
There's no fixed number — it depends on your individual stress response and how long the stress lasts. A few days to two weeks is common. In cases of severe or prolonged stress, your period can be absent for months (functional hypothalamic amenorrhoea). Your cycle typically returns to normal within 1-3 cycles once the stress resolves.
▸Can stress cause you to miss a period completely?
Yes. If cortisol levels remain elevated for long enough, ovulation can be suppressed entirely, resulting in a missed period. If you miss three or more consecutive periods, see your GP to rule out other causes like PCOS, thyroid conditions, or pregnancy.
▸How do I know if my late period is from stress or pregnancy?
Take a pregnancy test — it's the only reliable way to tell. Stress and early pregnancy share very similar symptoms (breast tenderness, fatigue, nausea, mood changes) because both involve progesterone fluctuations. A test is reliable from the day your period is due. If negative but still no period after a week, retest.
▸Does stress affect fertility?
Stress can affect fertility by delaying or preventing ovulation, which reduces the number of cycles in which conception is possible. However, moderate everyday stress is unlikely to prevent pregnancy on its own. The bigger concern is chronic, severe stress that consistently disrupts your cycle. Addressing stress through nutrition, sleep, and lifestyle changes can help restore normal ovulatory function.
You might also find helpful:
References
- Kolhe, J.V. et al. (2024). Bloody stressed! A systematic review of the associations between adulthood psychological stress and menstrual cycle irregularity. Neuroscience & Biobehavioral Reviews, 163, 105784. doi:10.1016/j.neubiorev.2024.105784
- Berga, S.L. & Loucks, T.L. (2006). Use of cognitive behavior therapy for functional hypothalamic amenorrhea. Annals of the New York Academy of Sciences, 1092, 114-129. doi:10.1196/annals.1365.010
- Gordon, C.M. et al. (2023). Functional hypothalamic amenorrhea: Recognition and management of a challenging diagnosis. Mayo Clinic Proceedings, 98(9), 1376-1387. doi:10.1016/j.mayocp.2023.05.014
- Meczekalski, B. et al. (2014). Functional hypothalamic amenorrhea and its influence on women's health. Journal of Endocrinological Investigation, 37(11), 1049-1056. doi:10.1007/s40618-014-0169-3
- Nagma, S. et al. (2015). To evaluate the effect of perceived stress on menstrual function. Journal of Clinical and Diagnostic Research, 9(3), QC01-QC03. doi:10.7860/JCDR/2015/6906.5611
- Bae, J. et al. (2018). Factors associated with menstrual cycle irregularity and menopause. BMC Women's Health, 18, 36. doi:10.1186/s12905-018-0528-x
- Toufexis, D. et al. (2014). Stress and the reproductive axis. Journal of Neuroendocrinology, 26(9), 573-586. doi:10.1111/jne.12179
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult a qualified healthcare professional before making changes to your diet, supplement routine, or health plan. If your period has been absent for three months or more, please see your GP.
All my Free Resources. No spam. Unsubscribe anytime.














