Spotting Before Period: Causes, What It Looks Like, and When It's a Sign of Pregnancy
What premenstrual spotting actually means, when it could signal pregnancy, and when to see a doctor — from a nutritionist who's been there.

Key Takeaways
- Spotting before your period is usually light pink or brown bleeding that doesn't need a pad — it's different from your actual period flow
- The most common cause is a normal progesterone drop in the late luteal phase, but hormonal birth control, ovulation, polyps, and early pregnancy can also cause it
- If you're trying to conceive, spotting 6–12 days after ovulation could be an early pregnancy sign — but most spotting before a period is not implantation bleeding
- See a doctor if spotting lasts more than 3 days before your period, happens every cycle, or comes with pain, heavy bleeding, or unusual discharge
You go to the bathroom, see a faint streak of pink or brown on the tissue, and your brain immediately starts running through possibilities. Is my period starting early? Could I be pregnant? Is something wrong?
I've been there — more times than I can count. During the months I was trying to conceive, every tiny spot of blood in those final days before my period was due sent me spiralling. Was it implantation? Was it my period arriving early again? After two chemical pregnancies, I became hyper-aware of every single thing my body did in that window.
So if you're staring at a panty liner right now wondering what that faint smudge means, I want you to know: you're not overthinking it. Spotting before your period is genuinely one of the most common — and most confusing — things your cycle can throw at you. And in most cases, there's a perfectly reasonable explanation.
What Counts as Spotting (and How It Differs From Your Period)
Spotting and your period might both involve blood, but they're not the same thing. Spotting is light bleeding that happens outside your regular menstrual flow — usually just a few drops that you notice on tissue or your underwear, not enough to fill a pad or tampon.
Colour matters here. Spotting before your period is typically light pink, rust-coloured, or brown. Brown spotting just means the blood is older — it's had time to oxidise before leaving your body. Bright red blood that increases in flow is more likely the start of your actual period.
Volume is the clearest difference. The average menstrual period produces 30–72ml of blood over 3–7 days. Spotting? Think a few drops to a teaspoon. If you need a pad or tampon, it's probably not spotting anymore — that's your period arriving.
Duration tells you something too. Premenstrual spotting usually lasts 1–2 days. If light bleeding stretches beyond 3 days before your period starts, that's worth mentioning to your doctor, because it can sometimes signal a shorter luteal phase — the second half of your menstrual cycle after ovulation.
Why You Might Spot Before Your Period
There isn't one single reason for spotting before your period — your body has a few different mechanisms that can produce light bleeding in that premenstrual window. Here are the most common causes, roughly in order of how likely they are.
Progesterone Dropping (The Most Common Reason)
After ovulation, your corpus luteum — the temporary structure left behind on your ovary — produces progesterone to maintain the lining of your uterus. If pregnancy doesn't happen, progesterone levels fall, and that decline triggers your endometrium to start breaking down. Your period follows.
But sometimes, progesterone drops slightly before your period is actually due, and a small amount of the uterine lining starts to shed early. Research from Kassem et al. (2020) found that women who experienced spotting before menstrual bleeding had higher progesterone metabolite levels during the luteal phase but a slower rate of decline — essentially, their bodies took longer to fully transition, creating a gradual "tailing off" rather than a clean start to their period.
This is completely normal in most cases. But if it happens consistently — spotting for more than 2–3 days before every period — it could indicate luteal phase deficiency (LPD), where progesterone support isn't quite sufficient to maintain the lining until your period properly begins. The ASRM (2021) notes that premenstrual spotting is one of the clinical signs associated with LPD, alongside a luteal phase shorter than 9 days.
Hormonal Birth Control
If you're on the combined pill, a progestogen-only pill, an IUD, or an implant, breakthrough bleeding is one of the most common side effects — especially in the first 3–6 months. Your body is adjusting to exogenous hormones, and the endometrium doesn't always behave predictably during that transition.
Missing a pill, taking it at inconsistent times, or running packs back-to-back can also trigger spotting. This doesn't usually mean anything is wrong — but if it's persistent or bothering you, it's worth discussing with your GP or prescriber.
Ovulation Spotting
Some women notice light spotting mid-cycle, around the time of ovulation. This happens when the rapid rise in oestrogen just before the egg is released causes a brief dip in endometrial stability. It's usually very brief — a few hours to a day — and often comes with one-sided pelvic twinges (mittelschmerz).
Mid-cycle spotting is different from premenstrual spotting in timing (day 12–16 vs day 24–28), but if your cycles are irregular, it can sometimes be hard to tell which is which. Tracking your cycle with an ovulation test or basal body temperature can help you pin down the timing.
Implantation Bleeding
This is the one everyone asks about. If a fertilised egg implants into the uterine lining — usually 6–12 days after ovulation — it can cause very light spotting. The timing often overlaps with when you'd expect premenstrual spotting, which is why it causes so much confusion.
I need to be honest with you about something, though. The evidence that implantation itself directly causes vaginal bleeding is actually weak. Harville et al. (2003) studied 151 clinical pregnancies prospectively and found that only 9% experienced any vaginal bleeding in the first 8 weeks — and the bleeding rarely coincided with the actual day of implantation. The researchers concluded they "found no support for the hypothesis that implantation can produce vaginal bleeding."
That doesn't mean spotting around the time of implantation never happens — it clearly does for some women. But it's probably less common than the internet would have you believe, and the mechanism may have more to do with the hormonal shifts of very early pregnancy than the physical act of the embryo burrowing in.
Cervical Causes
Cervical ectropion — where cells from the inside of the cervix appear on the outside — is common in women of reproductive age, especially those on hormonal birth control or during pregnancy. These cells bleed more easily, sometimes producing spotting after intercourse or in the days before your period. A StatPearls review (2023) notes that cervical ectropion is found in up to 55% of women using oral contraceptives.
Cervical polyps — small, benign growths on the cervix — can also cause intermenstrual spotting. They're harmless in most cases but worth having checked if spotting persists.
Uterine Polyps or Fibroids
Endometrial polyps are small overgrowths of the uterine lining that can cause bleeding between periods, heavy periods, or irregular bleeding. Dreisler et al. (2009) found that endometrial polyps appear in 6–32% of women with abnormal uterine bleeding, depending on the population studied. Fibroids — benign muscle growths in the uterine wall — can cause similar symptoms, particularly submucosal fibroids (those that press into the uterine cavity).
Both polyps and fibroids are usually diagnosed via ultrasound. If they're causing persistent spotting or affecting fertility, your healthcare provider may recommend removal — there's usually no cause for concern, but it's better to know what you're dealing with.
Thyroid or Other Hormonal Issues
Your thyroid gland quietly runs a lot of your reproductive function. Both hypothyroidism (underactive) and hyperthyroidism (overactive) can cause irregular bleeding, including spotting before your period. Sonntag and Ludwig (2012) note that thyroid dysfunction and hyperprolactinaemia are among the underlying hormonal disturbances that should be investigated when premenstrual spotting is recurrent.
Perimenopause — the transition phase before menopause — is another common cause, particularly for women over 40. Fluctuating oestrogen and progesterone levels create unpredictable bleeding patterns, and spotting before periods is often one of the first signs.
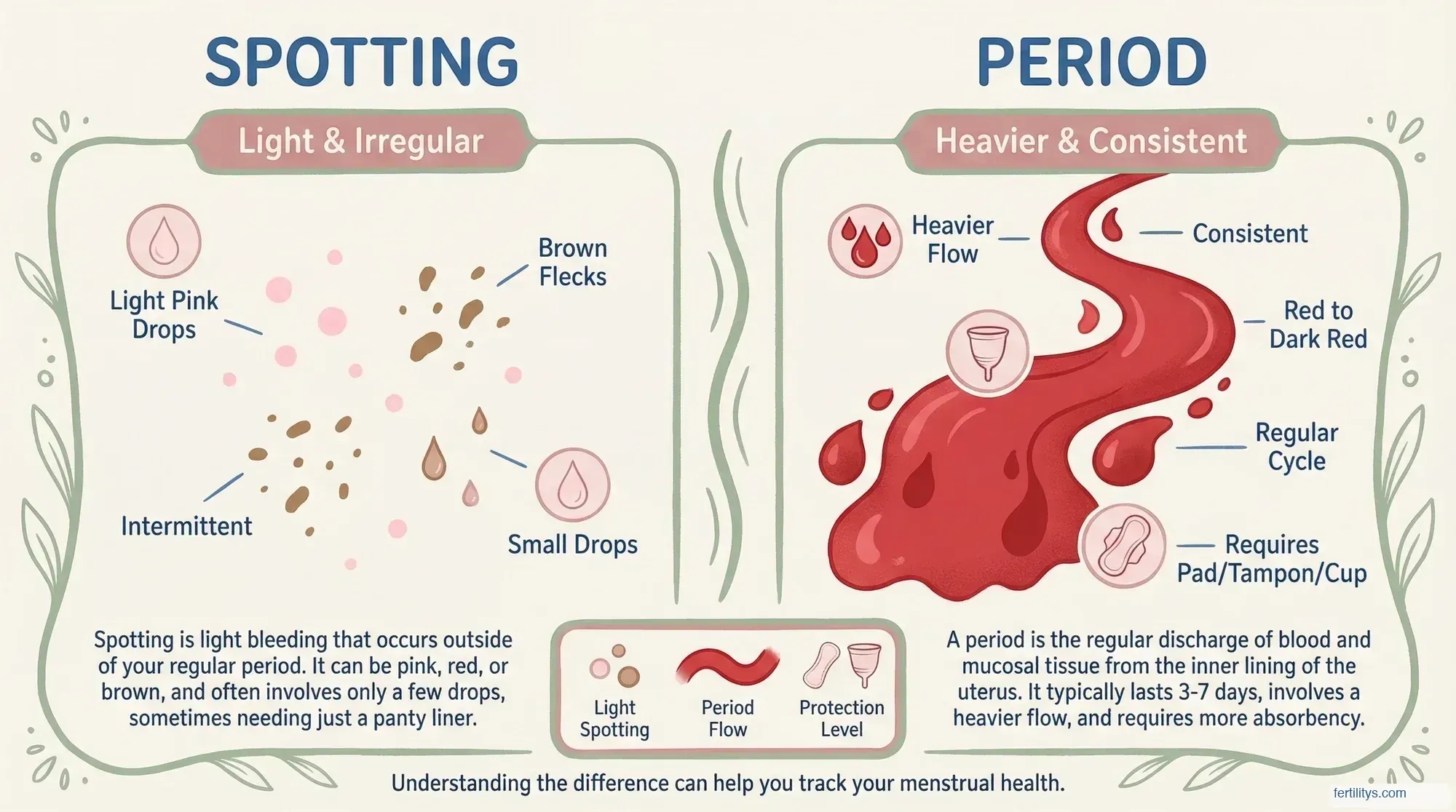
Spotting vs Period: How to Tell the Difference
When you're trying to work out whether what you're seeing is spotting or the start of your period, these are the things to look at:
| Feature | Spotting | Period |
|---|---|---|
| Colour | Light pink, brown, or rust | Bright red, darkening to brown |
| Flow | A few drops — panty liner at most | Needs a pad, tampon, or cup |
| Duration | 1–2 days | 3–7 days |
| Clots | None | Common, especially days 1–2 |
| Cramping | Mild or absent | Often moderate to strong |
| Pattern | Intermittent, on and off | Builds, peaks, then tapers |
| When it starts | 1–3 days before period due | On your expected period date |
A practical test: if you can wipe it away and it doesn't come back for hours, that's spotting. If it keeps coming and you're reaching for protection, your period has started.

Is This Spotting a Sign of Pregnancy?
If you're actively trying to conceive, this is probably the question burning in your mind. And I wish I could give you a definitive answer, but the honest truth is: spotting alone can't tell you whether you're pregnant.
Here's what we do know. About 25% of women experience some vaginal bleeding in the first trimester of pregnancy (AAFP, 2019). The good news from the Harville et al. (2003) study is that nearly all women who experienced early bleeding in their research went on to have successful pregnancies — 12 out of 14.
Spotting that might suggest early pregnancy typically looks like this:
- Very light — a few spots, usually pink or brown
- Occurs 6–12 days after ovulation (roughly 8–10 DPO is most common)
- Lasts a few hours to 1–2 days, then stops completely
- May come with very mild cramping — different from your usual period cramps
- Your period doesn't arrive on schedule after the spotting stops
Spotting that's more likely your period approaching:
- Transitions from light to heavier flow within 24–48 hours
- Becomes bright red
- Comes with your typical premenstrual symptoms (bloating, mood changes, breast tenderness)
- Follows your normal cycle pattern
If you think there's a chance you could be pregnant, the only reliable way to know is to take a pregnancy test. Wait until the day your period is due — or ideally a day or two after — for the most accurate result. Testing too early can give you a false negative because hCG levels may not be high enough to detect yet. I go into this in more detail in my guide to when to take a pregnancy test.
I'll be honest — during my own journey, I drove myself mad analysing every spot of blood during the two-week wait. After my two chemical pregnancies, I'd learned that early spotting could mean anything. The only thing that actually gave me an answer was the test. Everything else was just my brain trying to solve a puzzle that didn't have enough pieces yet.
When to See a Doctor
Most premenstrual spotting is harmless. But there are situations where it's worth getting checked — not because something is definitely wrong, but because it's better to rule things out than to worry.
Book an appointment if:
- You spot before every period and it lasts 3+ days
- Spotting started recently and you can't explain why (no new medication, no change in routine)
- You're also experiencing heavy periods, pain during sex, or unusual vaginal discharge
- You've been trying to conceive for 6+ months without success and you notice regular luteal phase spotting
- You're over 40 and your bleeding patterns have changed
- Spotting occurs after menopause (any post-menopausal bleeding needs investigation)
Go urgently if:
- You have heavy bleeding with severe pain (possible ectopic pregnancy or miscarriage if you could be pregnant)
- You feel dizzy or faint alongside bleeding
- You have a positive pregnancy test and then start bleeding
Your doctor will likely ask about your cycle length, when the spotting happens, and whether you're on any hormonal medication. They may suggest blood tests (progesterone, thyroid function, prolactin) or an ultrasound to check for polyps or fibroids. If you're tracking your cycle — which I always recommend — bring your data with you. It makes the conversation much more productive.
The Bottom Line
Spotting before your period is one of those things that can mean everything or nothing — and the uncertainty is the hardest part, especially when you're trying to conceive. But here's what I want you to take away from this.
Most premenstrual spotting is caused by the natural drop in progesterone that happens at the end of every menstrual cycle. It's your body transitioning, not malfunctioning. If spotting is brief, light, and doesn't happen every single cycle, it's almost certainly nothing to worry about.
If it does happen every cycle, lasts more than a couple of days, or comes with other symptoms — get it checked. Not because it's probably serious, but because you deserve to understand what your body is doing. A simple blood test or ultrasound can give you answers and, more importantly, peace of mind.
▸Is spotting before my period normal?
Yes, in most cases. Light spotting 1–3 days before your period is a common result of falling progesterone levels. It's only worth investigating if it happens every cycle, lasts more than 3 days, or comes with other symptoms like pain or heavy bleeding.
▸Does spotting before my period mean I'm pregnant?
It can be an early sign of pregnancy if it occurs 6–12 days after ovulation and stops within 1–2 days. But most premenstrual spotting is not related to pregnancy. The only way to know for sure is to take a pregnancy test once your period is due.
▸Does spotting before my period mean low progesterone?
Not necessarily. Some spotting before your period is a normal part of the progesterone withdrawal that triggers menstruation. But if you consistently spot for 3+ days before every period and your luteal phase is shorter than 10 days, it could indicate luteal phase deficiency — a condition your doctor can test for with a mid-luteal progesterone blood test.
▸What colour is spotting before a period?
Premenstrual spotting is usually light pink, rust-coloured, or brown. Brown spotting simply means the blood is older and has oxidised before leaving the body. Bright red bleeding that gets heavier is more likely the start of your actual period rather than spotting.
▸How long does spotting before a period last?
Typically 1–2 days. Some women notice a few hours of light spotting the day before their period starts — that's completely normal. If spotting lasts 3 or more days before your period begins, or if the pattern is new for you, it's worth discussing with your doctor.
▸Does spotting before my period count as day 1 of my cycle?
No. Day 1 of your cycle is the first day of full menstrual flow — blood that needs a pad, tampon, or cup. Light spotting in the days before doesn't count. This distinction matters particularly if you're tracking your cycle for fertility purposes or timing ovulation tests.
You might also find helpful:
References
- Kassem A, Miksztal A, Guo R, Wactawski-Wende J, Mumford SL, Schisterman EF, et al. Hormonal profiles of menstrual bleeding patterns during the luteal-follicular transition. J Clin Endocrinol Metab. 2020;105(5):e2024-e2033. doi:10.1210/clinem/dgaa109
- Practice Committee of the American Society for Reproductive Medicine. Diagnosis and treatment of luteal phase deficiency: a committee opinion. Fertil Steril. 2021;115(6):1416-1423. doi:10.1016/j.fertnstert.2021.02.031
- Harville EW, Wilcox AJ, Baird DD, Weinberg CR. Vaginal bleeding in very early pregnancy. Hum Reprod. 2003;18(9):1944-1947. doi:10.1093/humrep/deg379
- Henshaw SK. Unintended pregnancy and abortion: a public health perspective. In: Paul M, et al., eds. A Clinician's Guide to Medical and Surgical Abortion. Churchill Livingstone; 1999. Cited in: AAFP. First trimester bleeding: evaluation and management. Am Fam Physician. 2019;99(3):166-174.
- Dreisler E, Stampe Sørensen S, Ibsen PH, Lose G. Prevalence of endometrial polyps and abnormal uterine bleeding in a Danish population aged 20-74 years. Ultrasound Obstet Gynecol. 2009;33(1):102-108. doi:10.1002/uog.6259
- Sonntag B, Ludwig M. An integrated view on the luteal phase: diagnosis and treatment in subfertility. Clin Endocrinol (Oxf). 2012;77(4):500-507. doi:10.1111/j.1365-2265.2012.04464.x
- Cervical ectropion. StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023. NCBI Bookshelf
Medical disclaimer: This article is for informational purposes only and does not constitute medical advice. Always consult a qualified healthcare professional before making decisions about your health or treatment. I'm a registered nutritionist (MSc, RNutr), not a medical doctor.
⚕️ Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult a qualified healthcare professional before making decisions about your fertility or reproductive health.
All my Free Resources. No spam. Unsubscribe anytime.













