Key Takeaways
- The average true cost of one private IVF cycle is approximately £6,939 — but advertised prices often exclude medication, tests, and add-ons
- NHS funding depends on where you live. NICE recommends three cycles for women under 40, but most areas offer fewer
- Medication alone typically costs £1,000–£2,500 per cycle and is rarely included in clinic package prices
- Add-ons like ICSI (£1,375) and embryo freezing (£550) can push a single cycle above £8,000
- Cumulative success rates reach 65% after six cycles — so budgeting for one cycle only rarely tells the full story
I want to be honest with you about something: IVF costs in the UK are confusing on purpose. Clinics advertise headline prices that look manageable, then the actual bill arrives with extras you didn't know about — medication, blood tests, embryo freezing, ICSI. By the time you've added everything up, you're often paying thousands more than that initial quote suggested.
I know this because I sat in those consultation rooms myself. When my AMH came back at 3 — well below the 20+ expected for my age — clinics told me egg freezing was my only real option. Three rounds at £5,000–£7,000 each, with no guarantee any of it would work. That financial reality hit almost as hard as the diagnosis itself.
So this is the article I wish I'd had back then. Not a glossy breakdown from a clinic's marketing team, but an honest look at what fertility treatments actually cost in 2026 — NHS and private, the fees they don't mention upfront, and practical ways to make it more affordable.
What Does a Single IVF Cycle Actually Cost?
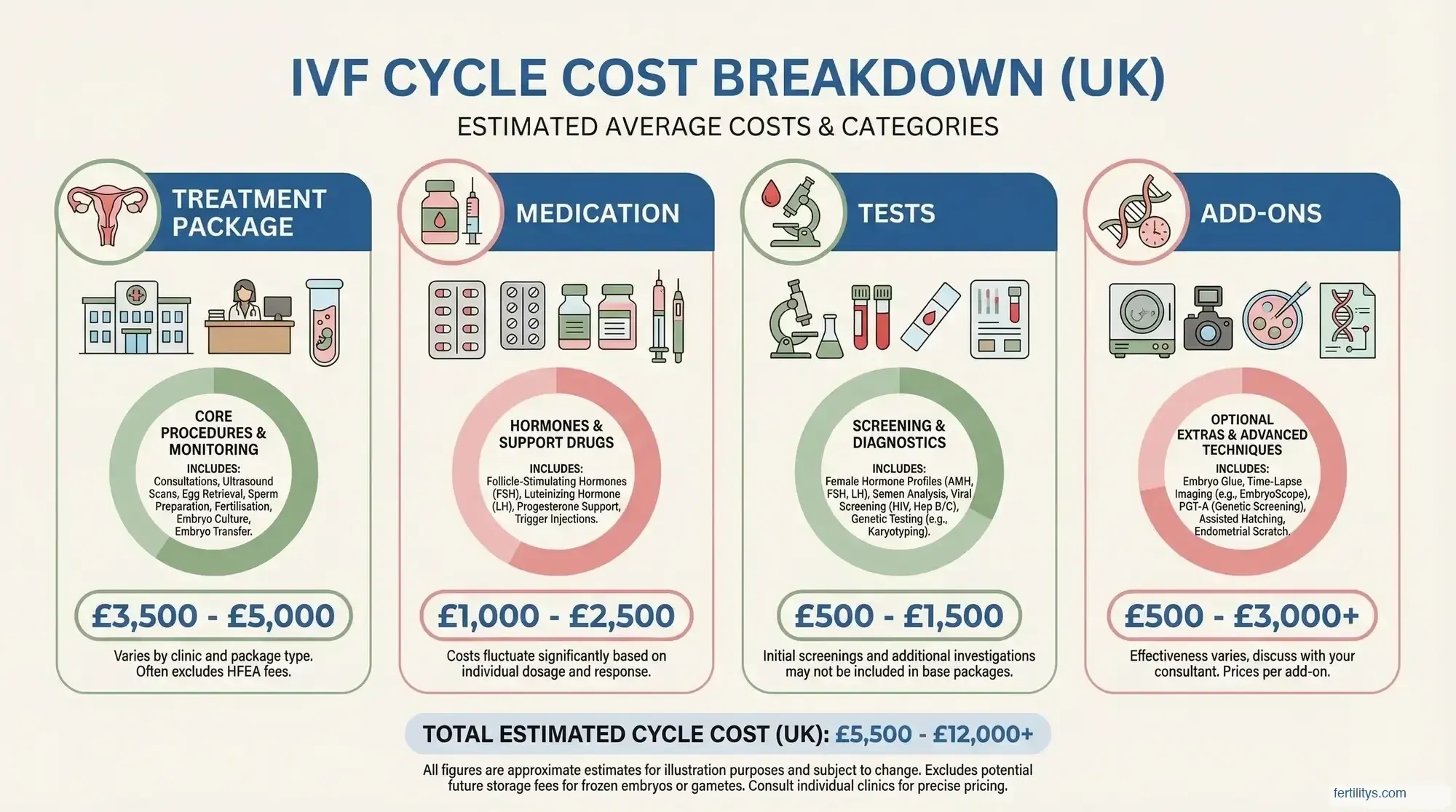
The short answer: somewhere between £5,000 and £10,000 for one complete cycle, depending on your clinic, your location, and what extras are included. But that range is deliberately unhelpful, so let me break it down properly.
According to data from Seen Fertility's analysis of UK fertility clinics, the average true cost of one IVF cycle in 2025–26 is £6,939 — that's the treatment package plus medication. The package alone averages £4,890, but medication (which is almost never included in advertised prices) adds another £1,500 on average (Seen Fertility, 2026).
Here's what makes those headline prices misleading. A clinic might advertise "IVF from £3,500" — and that's technically true. But it only covers the core procedure: consultations, egg collection, embryo transfer, and lab time. Everything else is extra.
| Cost Component | Average Cost (2025–26) | Range |
|---|---|---|
| IVF treatment package | £4,890 | £3,500–£14,000 |
| Pre-treatment tests (both partners) | £549 | £300–£900 |
| Medication | £1,500 | £1,000–£2,500 |
| Sedation (egg collection) | £300 | £150–£500 |
| Embryo freezing | £550 | £350–£1,000 |
| Typical total (no add-ons) | £6,939 | £5,000–£7,500 |
And that's before add-ons. Which brings us to one of the most controversial parts of IVF pricing.
IVF Add-Ons: What They Cost and Whether They're Worth It
If you've started researching clinics, you've probably already encountered the word "add-ons." These are optional procedures your clinic might recommend alongside standard IVF — things like ICSI, embryo glue, endometrial scratching, or PGT-A genetic testing.
Some are genuinely useful for specific situations. Others have limited evidence behind them. The HFEA uses a traffic light system to rate add-ons by evidence level — and most sit at amber (conflicting evidence) or red (no evidence of benefit).
ICSI — intracytoplasmic sperm injection, where a single sperm is injected directly into the egg — is the most common add-on and averages £1,375. It's well-established for male factor infertility, but some clinics recommend it routinely even when sperm quality is normal. If your partner's semen analysis is fine, ask your clinic why they're recommending it.
PGT-A (preimplantation genetic testing for aneuploidy) screens embryos for chromosomal abnormalities before transfer. It typically costs £2,000–£3,500 on top of your IVF cycle. The HFEA rates it as grey for women over 37 — meaning there's not enough evidence to confirm it improves live birth rates. For younger women, the evidence is even less clear. Harper et al. (2022) found that while PGT-A can reduce miscarriage rates in some populations, its benefit for cumulative live birth rates remains debated (PMC8995402).
| Add-On | Average Cost | HFEA Rating | When It Might Be Useful |
|---|---|---|---|
| ICSI | £1,375 | Green (for male factor) | Male factor infertility, previous fertilisation failure |
| Blastocyst culture | £550 | Green | Multiple embryos — helps select the strongest |
| Embryo glue | £275 | Amber | May help implantation — limited evidence |
| Endometrial scratch | £300 | Red | Previously recommended, now shown to have no benefit |
| PGT-A | £2,000–£3,500 | Grey (over 37) | Recurrent miscarriage, older age groups |
| Time-lapse imaging | £500–£850 | Amber | May aid embryo selection — unclear benefit |
I always tell my clients: before saying yes to any add-on, check the HFEA traffic light rating and ask the clinic for the specific evidence. A good clinic won't pressure you. And if they can't explain why they're recommending something for your particular case, that's a red flag.
NHS IVF: Who Qualifies and What You Actually Get
Here's where it gets properly frustrating. The NICE clinical guideline (CG156) recommends that women under 40 should be offered three full cycles of NHS-funded IVF after two years of trying to conceive. Women aged 40–42 who haven't previously had IVF should be offered one cycle, provided certain criteria are met (NICE, 2013).
But NICE guidelines are recommendations, not rules. In England, each local Integrated Care Board (ICB) decides independently how many cycles to fund — and whether to fund any at all. The result is what Fertility Network UK calls the "postcode lottery": where you live determines what treatment you can access.
In practice, this means:
- Some ICBs offer three cycles (matching NICE guidance) — but this is rare
- Most offer one or two cycles
- A handful offer none at all
- The definition of "one cycle" varies — in some areas it includes frozen embryo transfers from that stimulation; in others, it means one fresh transfer only
Scotland, Wales, and Northern Ireland have national policies rather than the regional approach used in England:
- Scotland: Up to three cycles for eligible patients, managed nationally — generally the most generous in the UK
- Wales: Two cycles for those meeting eligibility criteria
- Northern Ireland: One fresh cycle (historically underfunded compared to the rest of the UK)
"The postcode lottery genuinely kept me up at night. I had clients who'd moved house specifically to fall under a different ICB — uprooted their entire lives for one extra funded cycle. That shouldn't be how healthcare works."
Common eligibility criteria across most ICBs include age limits (typically under 40 for funded treatment, though this varies), BMI requirements (usually 19–30), non-smoker status, and a minimum period of trying to conceive (12–24 months of unprotected intercourse). Same-sex couples and single women may need to self-fund a number of intrauterine insemination (IUI) cycles before qualifying for NHS IVF.
It's also worth knowing that fertility preservation — egg freezing, for example — follows a separate funding pathway. Most NHS areas don't fund elective egg freezing, though medical fertility preservation before cancer treatment is usually covered.
If you're unsure about your area, the GOV.UK ICB funding page has a searchable list of policies by area, updated as of September 2025.
How Many Cycles Should You Budget For?
This is the question nobody wants to ask — because the honest answer is uncomfortable. A single IVF cycle gives you roughly a 1-in-3 chance of a live birth if you're under 35. But most people don't get pregnant on their first cycle.
A landmark study by Smith et al. (2015), published in JAMA, followed 156,947 UK women across 257,398 IVF cycles. They found that the cumulative prognosis-adjusted live birth rate reached 65.3% after six cycles for all women — and 68.4% for women under 40 using their own eggs (doi:10.1001/jama.2015.17296).
What does that mean in money terms? If you're budgeting for private IVF at ~£7,000 per cycle:
| Scenario | Estimated Total Cost | Cumulative Live Birth Rate (under 40) |
|---|---|---|
| 1 cycle | £7,000 | ~32% |
| 2 cycles | £14,000 | ~49% |
| 3 cycles | £21,000 | ~58% |
| 6 cycles | £42,000 | ~68% |
For women aged 40–42, success rates drop significantly — the first-cycle live birth rate falls to about 12%, with a cumulative rate of 31.5% after six cycles (Smith et al., 2015). Over 42, rates fall below 4% per cycle with own eggs, and donor egg IVF becomes the more realistic option.
The latest HFEA data (2025) shows that in 2023, 52,400 patients had over 77,500 IVF cycles at licensed UK clinics — approximately 1 in 32 UK births now comes from IVF (HFEA, 2025). That's roughly one child in every classroom. IVF is no longer unusual — but it remains expensive.
Practical Ways to Reduce What You Pay
I'm not going to pretend there's a hack that makes IVF cheap. There isn't. But there are genuine ways to bring the cost down:
Shop around on medication. Your clinic's pharmacy is usually the most expensive option. Once you have your prescription, compare prices at Asda (which sells fertility drugs at cost price), Fertility2U, and IVFPharmacy. Some patients save £300–£500 per cycle just by buying medication elsewhere. Your clinic may charge a small prescription fee (average £53), but it's usually worth it.
Ask about multi-cycle packages. Some clinics offer discounted rates if you commit to two or three cycles upfront. Given that most people need more than one cycle, this can reduce the per-cycle cost by 10–20%. But read the terms carefully — some packages are non-refundable even if you get pregnant on the first cycle.
Consider refund programmes. Companies like Access Fertility offer packages where you pay a fixed amount upfront for multiple cycles and get a partial or full refund if you don't achieve a live birth. These cost more than paying per cycle individually, but they cap your financial risk. They work best for younger patients with good prognosis — which is also who's most likely to succeed on fewer cycles. It's a trade-off.
Check your employer benefits. A growing number of UK employers now include fertility benefits in their healthcare packages — particularly in tech, finance, and large corporates. It's worth asking HR even if it's not advertised.
Explore clinical trials. The HFEA's Choose a Fertility Clinic tool can help you find clinics running research trials. Participating in a trial sometimes means free or reduced-cost treatment, though eligibility criteria can be strict.

The Emotional Cost Nobody Talks About
I can't write about IVF costs without talking about this. The financial pressure of IVF doesn't exist in isolation — it compounds an already emotionally brutal process.
A 2026 report from Fertility Network UK found that 42% of people going through fertility treatment feel suicidal, 90% report depression, and 70% experience relationship difficulties (Taylor & Francis, 2026). Financial strain is consistently cited as one of the top three stressors, alongside treatment failure and relationship impact.
When you're remortgaging your house, borrowing from family, or choosing between another cycle and a year of living expenses — the weight of that is enormous. And it affects treatment decisions in ways it shouldn't have to. I've worked with clients who've rushed into cycles before they were physically or emotionally ready, purely because they couldn't afford to wait.
If you're feeling that pressure right now, please know: taking time between cycles to recover — physically, emotionally, financially — is not wasted time. Your body needs that space to respond well to treatment.
The Bottom Line
IVF in the UK costs between £5,000 and £10,000 per cycle privately, with the true average sitting around £6,939 when you include medication and tests. NHS funding exists but varies wildly by location — and most areas fall short of NICE's recommendation of three cycles.
The most important thing I can tell you about IVF costs is this: get a fully costed treatment plan before you commit to any clinic. Not the headline price. Not the "starting from" figure on their website. The actual total — including tests, medication, sedation, embryo freezing, and any recommended add-ons. Then compare that number across at least three clinics.
And if you're at the stage where IVF is being discussed, please don't skip the preparation work. Optimising your nutrition, managing stress, and supporting your egg quality in the months before treatment can genuinely improve your chances — which means potentially fewer cycles and lower total costs. That's not wishful thinking; it's what the research shows, and it's what I built my entire practice around.
▸How much does one cycle of IVF cost in the UK?
The average true cost of one IVF cycle is approximately £6,939, which includes the treatment package (~£4,890) and medication (~£1,500). Costs range from £5,000 to over £10,000 depending on your clinic, location, and whether add-ons like ICSI are needed.
▸Can I get IVF for free on the NHS?
It depends on where you live. NICE recommends three funded cycles for women under 40, but each Integrated Care Board in England sets its own criteria. Some areas offer three cycles, many offer one or two, and a few offer none. Scotland, Wales, and Northern Ireland have separate national policies. Check your local ICB's fertility policy or use the GOV.UK NHS IVF funding page.
▸Why is IVF so expensive in the UK?
IVF involves specialist consultants, laboratory facilities, embryologists, anaesthetists, and expensive hormonal medications. Clinics are private healthcare providers and set their own prices — there's no regulation on what they can charge. The variation between clinics (£3,500 to £14,000 for a basic package) reflects differences in overheads, location, and how they package their services.
▸How many IVF cycles does it take to get pregnant?
There's no single answer, but research by Smith et al. (2015) in JAMA found that cumulative live birth rates for women under 40 reached 68.4% after six cycles. The first cycle gives roughly a 32% chance. Most fertility specialists recommend budgeting for at least two to three cycles when planning privately.
▸Are IVF add-ons worth paying for?
Some are, depending on your situation. ICSI is well-evidenced for male factor infertility. Blastocyst culture has good support. But many add-ons — including endometrial scratching and embryo glue — have limited or no evidence of improving live birth rates. Always check the HFEA's traffic light ratings before agreeing to any extras, and ask your clinic to explain why they're recommending a specific add-on for your case.
You might also find helpful:
References
- HFEA (2025). Fertility Treatment 2023: Trends and Figures. Human Fertilisation and Embryology Authority. Available at: hfea.gov.uk
- Smith, A.D.A.C. et al. (2015). Live-birth rate associated with repeat in vitro fertilisation treatment cycles. JAMA, 314(24), 2654–2662. doi:10.1001/jama.2015.17296
- NICE (2013). Fertility Problems: Assessment and Treatment. Clinical Guideline CG156. National Institute for Health and Care Excellence. nice.org.uk
- Seen Fertility (2026). How Much Does IVF Cost in the UK? Updated February 2026. seenfertility.com
- HFEA (2026). Treatment Add-Ons Traffic Light Rating System. hfea.gov.uk
- Harper, J. et al. (2022). The efficacy of add-ons: selected IVF add-on procedures and future directions. Journal of Assisted Reproduction and Genetics. PMC8995402
- Fertility Network UK / Taylor & Francis (2026). Lack of psychological support for those dealing with infertility in the UK. taylorandfrancisgroup.com
⚕️ Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult a qualified healthcare professional before making decisions about fertility treatment. Individual circumstances vary — your GP or fertility consultant can provide guidance tailored to your specific situation. Fertilitys is not a medical provider and does not offer diagnoses or treatment recommendations.
All my Free Resources. No spam. Unsubscribe anytime.














