There's a moment — usually a day or two after your period ends — when something shifts. The cramps stop. The fatigue lifts. You wake up and actually want to get out of bed. Your brain feels sharper. Your mood feels lighter. And if you've never paid much attention to your menstrual cycle beyond tracking your period, you might not realise this shift has a name.
It's your follicular phase. And it's doing a lot more than you think.
💡 Quick Answer
The follicular phase runs from day 1 of your period until ovulation — typically 10 to 16 days. Rising oestrogen drives higher energy, improved mood, changing cervical mucus, and growing follicles that prepare your body to release an egg.
What Is the Follicular Phase?
So what is the follicular phase, exactly? It's the first half of your menstrual cycle, spanning from the first day of your period right through to ovulation. If your cycle were a story, this would be the build-up — the part where your body gathers momentum, prepares an egg, and gets everything ready for a potential pregnancy.
Here's what's actually happening inside you during the follicular phase of the menstrual cycle. Your brain's pituitary gland releases follicle-stimulating hormone (FSH), which tells your ovaries to start developing follicles — small fluid-filled sacs, each containing an immature egg. Typically, between 5 and 20 follicles begin growing, though only one will eventually become the "dominant" follicle that reaches maturity (Reed & Carr, 2018).
As these follicles grow, they produce increasing amounts of oestrogen — specifically oestradiol (E2). This rising oestrogen is the driving force behind most of the symptoms during the follicular phase you'll notice: the energy boost, the mood lift, the changes in your cervical mucus, and the thickening of your uterine lining in preparation for potential implantation. Understanding the follicular phase of the menstrual cycle means understanding how oestrogen levels climb from their lowest point (during your period) to their peak (just before ovulation) — and how that climb affects everything from your energy levels to your skin.
Think of it this way: your period is the reset. The follicular phase is the rebuild.
How Long Is the Follicular Phase?
You'll often see "14 days" quoted as the standard follicular phase length. But that number is misleading — it assumes a perfectly regular 28-day cycle, which only about 13% of women actually have (Fehring et al., 2006).
In reality, the follicular phase is the most variable part of your cycle. While the luteal phase (the second half, after ovulation) stays relatively consistent at around 12 to 14 days, the follicular phase can range from as short as 10 days to as long as 21 days or more (Lenton et al., 1984).
What affects how long yours lasts?
- Age: Women in their late 30s and 40s tend to have shorter follicular phases. A study of 293 ovulatory cycles found that follicular phase length decreased significantly with age, driven by higher early-cycle FSH levels that accelerate follicle recruitment (Lenton et al., 1984).
- Stress: Chronic stress can delay ovulation, stretching the follicular phase out. Your body essentially pauses the process when cortisol levels are elevated (Wirth et al., 2011).
- Weight and nutrition: Both very low body weight and obesity can alter hormone signalling, affecting how quickly (or slowly) a dominant follicle emerges.
- PCOS: Women with polycystic ovary syndrome often have prolonged follicular phases because multiple follicles compete without one becoming dominant.
If your cycles vary in length — say, 26 days one month and 32 the next — it's almost certainly the follicular phase that's changing, not the luteal phase. This is completely normal and doesn't automatically mean something is wrong.
The Hormones Behind Your Follicular Phase Symptoms
Every symptom you experience during the follicular phase traces back to two hormones working in concert: FSH and oestrogen. Understanding their pattern helps you make sense of what your body's doing — and why you feel the way you do at different points in this phase.
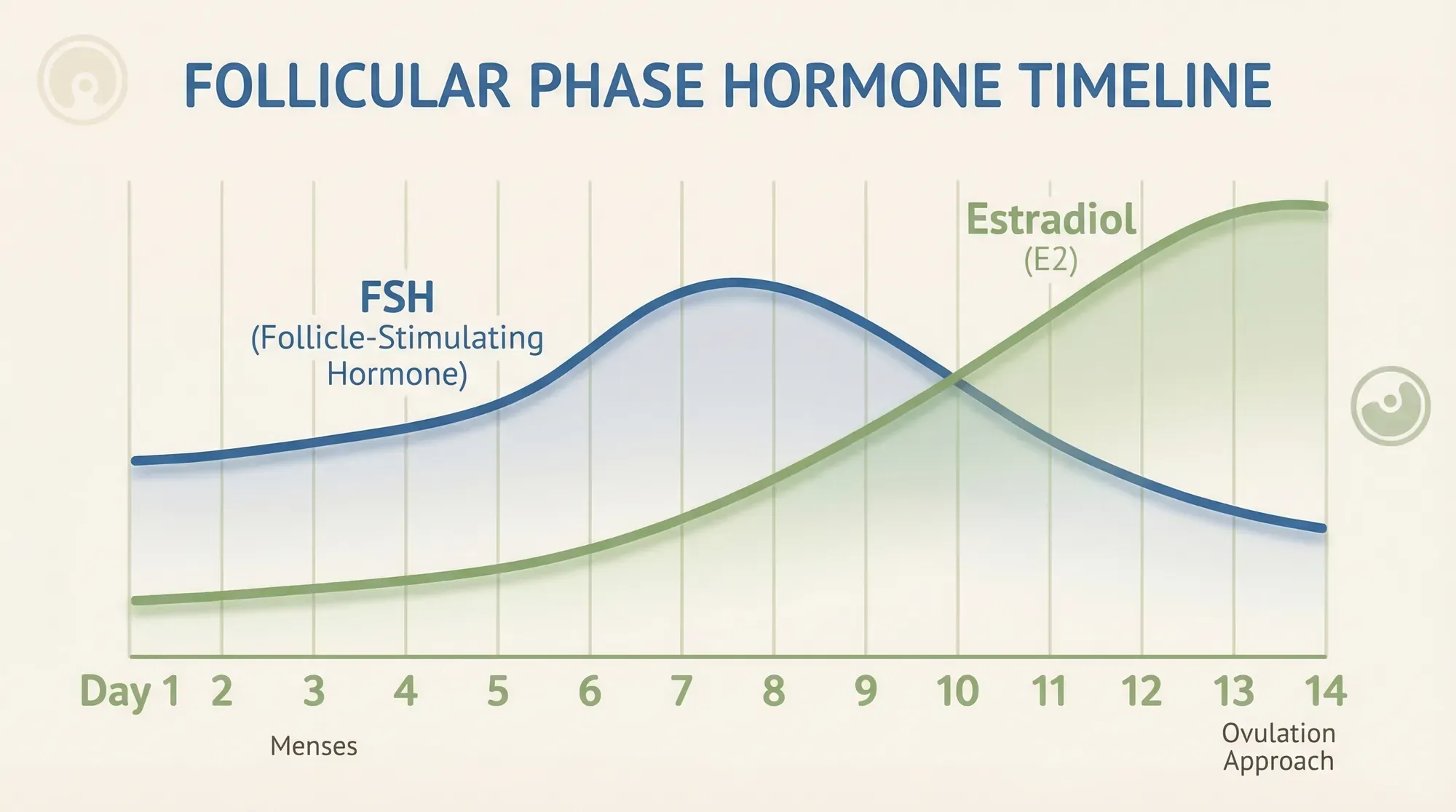
Early follicular phase (days 1–5, during your period): Oestrogen and progesterone are both at their lowest. FSH starts to climb, kickstarting follicle development. This is when you're still dealing with period symptoms — cramps, fatigue, possibly low mood. Your body is simultaneously shedding the old uterine lining and beginning to build the next cycle's foundation.
Mid-follicular phase (days 6–10): Oestrogen begins rising noticeably as the growing follicles produce more oestradiol. This is typically when you feel the "switch" — energy returning, mood brightening, mental clarity improving. FSH starts to level off as the dominant follicle takes over.
Late follicular phase (days 11–14+): Oestrogen hits its peak just before ovulation, triggering the LH surge that causes the dominant follicle to release its egg. You're likely feeling your best — highest energy, highest confidence, most fertile cervical mucus. Libido often peaks here too, which makes biological sense (Roney & Simmons, 2013).
The granulosa cells lining the dominant follicle also produce inhibin B, which feeds back to the pituitary gland and suppresses FSH — preventing the other follicles from developing further. By the time you ovulate, one follicle has "won" and the rest gradually break down (Macklon & Fauser, 2001).
Follicular Phase Symptoms: What You'll Actually Feel
Not every woman experiences every symptom, and the intensity varies between individuals and even between cycles. The physical symptoms, emotional shifts, and bodily changes all trace back to that same hormone pattern. But here's what rising oestrogen typically brings during the follicular phase:
Energy and Mood
This is the symptom most women notice first. After the fatigue and heaviness of menstruation, the follicular phase often feels like someone's flipped a switch. You sleep better. You wake up more easily. Your motivation returns.
There's solid science behind it. Oestrogen increases serotonin availability in the brain — the neurotransmitter linked to mood regulation and feelings of wellbeing (Amin et al., 2005). It also enhances dopamine activity, which affects motivation and reward processing. This is why the follicular phase can feel like your "productive" time — you're not imagining it, your neurochemistry is genuinely different.
A 2025 study in Biology confirmed that cognitive performance, particularly verbal fluency and processing speed, varied across the menstrual cycle, with measurable differences tied to hormone fluctuations (Schmalenberger et al., 2025). And while the research is nuanced — some studies find minimal differences at rest — the real-world experience of millions of women consistently describes the follicular phase as a time of increased mental sharpness.
That said, the very early follicular phase (days 1–3) is still a low-energy window. The boost comes after bleeding eases, typically around day 4 or 5. Don't expect to feel amazing on day 1 — you're still in the hormonal basement at that point.
Cervical Mucus Changes
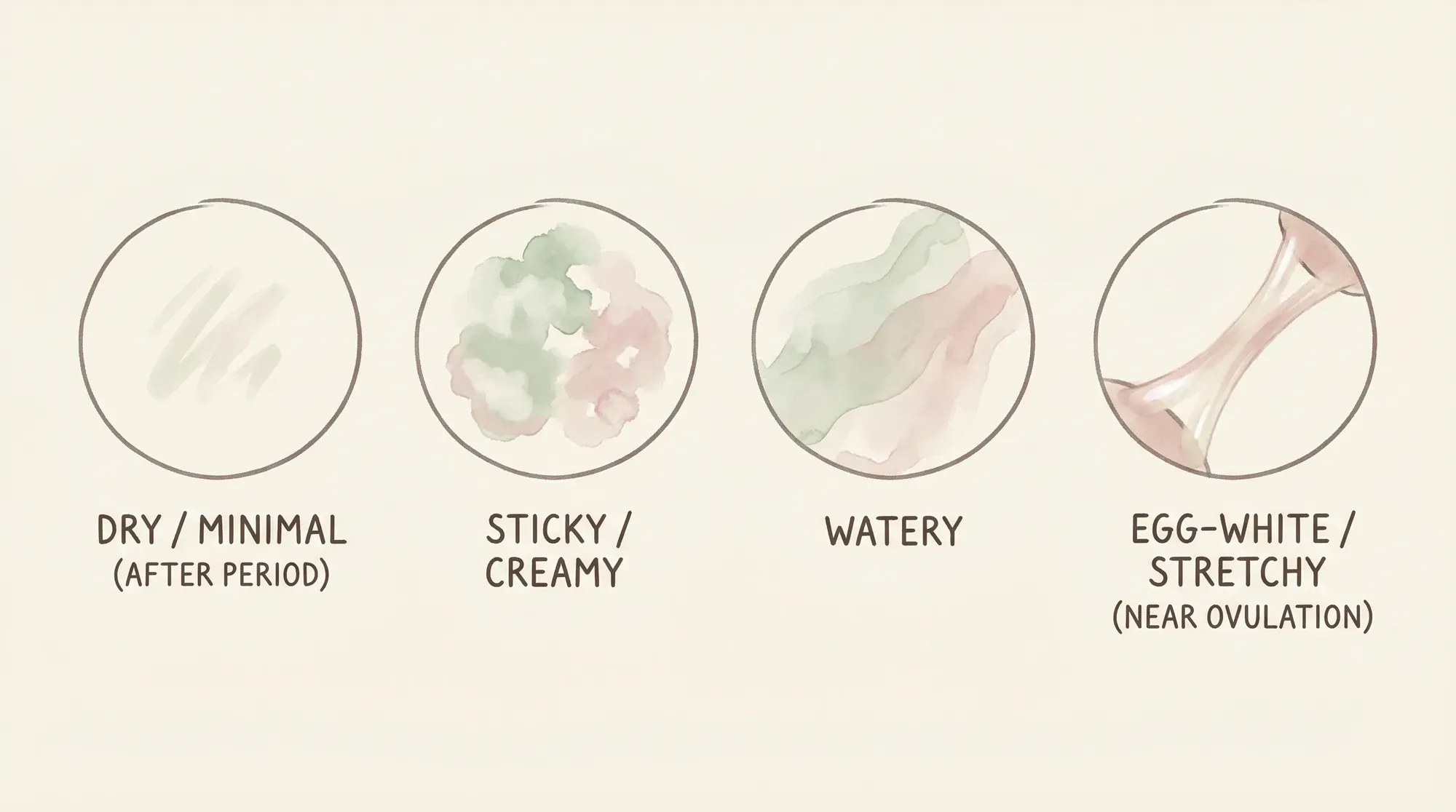
Follicular phase discharge follows a predictable pattern that's directly controlled by oestrogen, and tracking it is one of the most reliable ways to understand where you are in your cycle.
Right after your period, you might notice very little cervical mucus — a "dry" phase. As oestrogen rises through the mid-follicular phase, mucus becomes thicker and creamy or sticky. Then, as you approach ovulation in the late follicular phase, it transforms into what's often described as "egg-white" cervical mucus (EWCM) — clear, stretchy, slippery, and very slick.
This isn't random. The egg-white consistency has a specific biological purpose: it creates channels that help sperm swim through the cervix and survive for up to five days inside the reproductive tract (Bigelow et al., 2004). If you're trying to get pregnant, this is the mucus pattern that signals your most fertile window.
Physical Changes
Rising oestrogen affects more than your mood and mucus. You might also notice:
- Clearer skin: Oestrogen has an anti-inflammatory effect on the skin and helps regulate sebum production. Many women notice their skin looks its best in the late follicular phase — fewer breakouts, more "glow." This reverses in the luteal phase when progesterone rises and can trigger oiliness and acne.
- Breast tenderness easing: If your breasts felt heavy or sore during your period or late luteal phase, the follicular phase usually brings relief. Progesterone (the main driver of breast tenderness) is at its lowest.
- Increased libido: Oestrogen and a small rise in testosterone around mid-cycle often boost sex drive. Roney and Simmons (2013) found that women's self-reported sexual desire increased as oestradiol levels rose, independent of relationship status.
- Less bloating: Without the water-retention effects of progesterone, many women feel physically "lighter" during the follicular phase.
- Basal body temperature stays low: Your BBT remains relatively stable and low (around 36.1–36.4°C / 97.0–97.6°F) throughout the follicular phase. The temperature spike that indicates ovulation hasn't happened yet.
Mood Swings and Emotional Shifts
Despite the general upward trend in mood, the follicular phase isn't immune to emotional fluctuation — especially in the early days. The transition from the late luteal phase (when both oestrogen and progesterone drop sharply) into menstruation can bring irritability, tearfulness, or low mood that lingers into the first few days of the follicular phase.
For women with PMDD (premenstrual dysphoric disorder) or significant PMS, this crossover period can be the hardest. The mood boost typically kicks in around days 4–7 as oestrogen gains momentum, but it's not an overnight switch.
If your mood swings during the follicular phase feel extreme or unpredictable — particularly if they're interfering with work, relationships, or daily functioning — it's worth discussing with your GP. Cycle-related mood changes are real and treatable, and dismissing them as "just hormones" does women a disservice.
Follicular Phase Diet: What to Eat and Why It Matters
Your body has specific nutritional needs during the follicular phase — and meeting them can genuinely affect how you feel, how your hormones function, and how effectively your follicles develop.
Iron Replenishment
After menstruation, your iron levels are at their lowest. A 2025 study in Blood Advances confirmed that serum iron and transferrin saturation both drop during menses and the early follicular phase before gradually recovering (Mansour et al., 2025). The average woman loses 30–40ml of blood per period, and with it, valuable iron.
Prioritise iron-rich foods during the early follicular phase: red meat, lentils, spinach, fortified cereals, and tofu. Pair them with vitamin C (orange juice, red peppers, strawberries) to boost absorption. If you're a heavy bleeder, you may need more — about 1 in 5 women of reproductive age has low iron stores, and the follicular phase is when replenishment matters most.
Oestrogen-Supporting Foods
As your body produces more oestrogen, it also needs to metabolise it efficiently. Cruciferous vegetables — broccoli, cauliflower, Brussels sprouts, kale — contain compounds called glucosinolates that support healthy oestrogen metabolism through the liver (Higdon et al., 2007).
Lean proteins support follicle development and provide the amino acids needed for hormone production. Good choices during the follicular phase include:
- Wild salmon and sardines (omega-3s support follicle development and reduce inflammation)
- Eggs (choline supports cell division; the yolk contains vitamin D)
- Chicken and turkey (lean protein without excessive saturated fat)
- Lentils and chickpeas (iron + protein + fibre)

The Mediterranean Framework
If you want a simple framework for your follicular phase diet rather than a list of individual foods, the Mediterranean pattern is well-supported. A 2018 systematic review found that adherence to a Mediterranean diet was associated with better fertility outcomes, improved oestrogen metabolism, and lower inflammation markers (Karayiannis et al., 2018).
"I always come back to the Mediterranean diet as a foundation,"When I was navigating my own fertility journey — after that low AMH result of 3 at 32 — I didn't do anything extreme. I didn't cut out entire food groups or follow some complicated protocol. I focused on quality: wild fish two or three times a week, loads of vegetables, berries, olive oil, and plenty of legumes. My food-first approach was one of the four pillars of the protocol I built for myself, and it's what I recommend to every client now. Your follicles are developing for months before ovulation — what you eat during the follicular phase is literally feeding the egg you'll release.
Exercise During the Follicular Phase
The follicular phase is when your body is best equipped for higher-intensity movement. Rising oestrogen improves muscle recovery, increases pain tolerance, and supports glycogen storage — all of which make exercise feel easier and more rewarding compared to the luteal phase.
Research supports this timing. A 2020 meta-analysis published in Sports Medicine found that strength training during the follicular phase may produce slightly greater gains in muscle strength compared to identical training in the luteal phase (McNulty et al., 2020). The mechanism isn't fully understood, but oestrogen's role in muscle repair and satellite cell activation likely contributes.
What does this mean practically?
- Early follicular (period days): Listen to your body. Gentle movement — walking, yoga, light stretching — is usually enough. Some women feel fine exercising normally through their period; others need to ease off. Neither is wrong.
- Mid to late follicular: This is your window for higher-intensity training if that's your thing — HIIT, heavy lifting, longer runs, challenging classes. Your body can handle more and will recover faster.
But a word of caution here. "I used to do intense HIIT sessions five or six times a week," Danielle shares. "When I started digging into the research during my fertility journey, I realised that level of intensity was driving my cortisol through the roof. I switched to gentler exercise — yoga, walking, lighter resistance work — and it was one of the changes I believe made a real difference to my hormone balance. The follicular phase gives you more energy for exercise, but that doesn't mean you should push to exhaustion every session. Work with your body, not against it."

When the Follicular Phase Is Too Short or Too Long
A "normal" follicular phase length falls roughly between 10 and 21 days. But what if yours sits outside that range?
Short Follicular Phase (Under 10 Days)
A consistently short follicular phase — under 10 days — can signal that follicles are being recruited and matured too quickly, which may affect egg quality. This pattern becomes more common with age as FSH levels rise. Lenton et al. (1984) found a clear inverse relationship between age and follicular phase length: older women's higher baseline FSH essentially rushes the process.
If you're trying to get pregnant and your follicular phase seems very short, mention it to your fertility specialist. It doesn't mean you can't conceive, but it's useful information for treatment planning.
Long Follicular Phase (Over 21 Days)
A prolonged follicular phase usually means ovulation is delayed. Common causes include stress, significant weight changes, thyroid dysfunction, PCOS, or coming off hormonal contraception. In most cases, the follicle does eventually mature and release — it just takes longer.
The concern with a very long follicular phase isn't the length itself but what it might indicate about ovulatory health. If your cycles regularly exceed 35 days, tracking ovulation (through cervical mucus, BBT, or OPKs) and discussing the pattern with your doctor is sensible.
The Follicular Phase and Getting Pregnant
If you're trying to conceive, understanding the follicular phase isn't just biology trivia — it's practically useful.
Your fertile window opens in the late follicular phase, approximately 5 days before ovulation through to the day of ovulation itself. A landmark 1995 study by Wilcox et al. found that virtually all pregnancies resulted from intercourse during this 6-day window, with the highest probability on the day before ovulation and ovulation day itself.
This means the follicular phase is when you want to start paying attention to fertility signs:
- Cervical mucus transitioning to egg-white consistency — your most reliable real-time fertility signal
- LH surge on ovulation predictor kits (OPKs) — typically 24–36 hours before ovulation
- Increased libido — your body's way of nudging you toward timed intercourse
- Mittelschmerz — a one-sided twinge or cramp some women feel around ovulation
The follicular phase is also when your oocyte (egg) goes through its final maturation stages. The nutritional and lifestyle choices you make during this phase — adequate iron, antioxidants, good sleep, manageable stress — directly support the quality of the egg that will be released. You can't change your ovarian reserve, but you can influence the environment in which your eggs develop.
The Bottom Line
The follicular phase is your body's rebuilding season. From the first day of your period through to ovulation, rising oestrogen drives a cascade of changes — higher energy, improved mood, evolving cervical mucus, developing follicles, and a thickening uterine lining. It's the phase where most women feel their most capable, and understanding its patterns gives you real power over your health and fertility decisions.
What varies — and this matters — is how long it lasts and how intensely you experience it. Your age, stress levels, nutrition, and general health all shape your follicular phase. There's no single "normal," and cycles that fluctuate by a few days are nothing to worry about.
Whether you're tracking your cycle for fertility, managing symptoms, or simply wanting to understand your body better, the follicular phase is worth paying attention to. It's doing more work than any other phase of your cycle — and once you know what to look for, you can support it.
Frequently Asked Questions
▸What are the most common symptoms during the follicular phase?
The most commonly reported symptoms during the follicular phase include increased energy, improved mood, changes in cervical mucus (progressing from dry to egg-white consistency near ovulation), reduced bloating, clearer skin, and higher libido. The early follicular phase (during your period) still involves menstrual symptoms like cramps and fatigue, but these typically ease by day 4 or 5 as oestrogen rises.
▸How long is the follicular phase supposed to last?
The follicular phase typically lasts between 10 and 21 days, with an average of about 14 days in a 28-day cycle. But it's the most variable part of the menstrual cycle — if your cycles differ in length month to month, it's almost always the follicular phase that's changing. Shorter follicular phases are more common as women age, driven by higher baseline FSH levels.
▸What does follicular phase discharge look like?
Follicular phase discharge changes throughout the phase. Right after your period, you may notice very little — a "dry" phase. As oestrogen rises, mucus becomes creamy or sticky. Near ovulation (late follicular phase), it becomes clear, stretchy, and slippery — often described as "egg-white" cervical mucus. This fertile-quality mucus helps sperm survive and travel through the cervix.
▸Is the follicular phase the best time to exercise?
For many women, yes. Rising oestrogen during the follicular phase supports better muscle recovery, improved glycogen storage, and higher pain tolerance — making exercise feel easier and potentially more effective. Research suggests strength training during the follicular phase may produce slightly greater gains than identical training in the luteal phase (McNulty et al., 2020). That said, the early days (during your period) may call for gentler movement.
▸Can you get pregnant during the follicular phase?
Yes — the fertile window begins in the late follicular phase. Sperm can survive up to five days in fertile cervical mucus, so intercourse in the days leading up to ovulation can result in pregnancy. The highest conception probability is on the day before and the day of ovulation itself (Wilcox et al., 1995). Tracking cervical mucus and using OPKs during the follicular phase helps identify this window.
▸What foods are best during the follicular phase?
Focus on iron-rich foods (red meat, lentils, spinach) to replenish stores lost during menstruation, paired with vitamin C for absorption. Cruciferous vegetables (broccoli, kale, cauliflower) support healthy oestrogen metabolism. Omega-3 rich fish (salmon, sardines), eggs, and legumes provide the protein and nutrients your developing follicles need. A Mediterranean dietary pattern offers a well-researched framework for follicular phase nutrition.
▸How long does the follicular phase last?
The follicular phase varies from 10-21 days, with an average of about 14 days. It's the most variable part of your cycle — stress, illness, and lifestyle changes primarily affect follicular phase length, which is why cycle length varies.
▸What should I eat during the follicular phase?
Focus on iron-rich foods (to replenish after menstruation), phytoestrogens (flaxseed, soy), lean proteins, and complex carbohydrates. This is a good time for nutrient-dense meals as your body prepares for ovulation.
▸Can the follicular phase be too short?
A follicular phase shorter than 10 days may not give a follicle enough time to mature properly. This can occasionally affect egg quality. If your cycles are consistently very short (under 24 days), mention it to your GP.
You might also find helpful:
References
- Reed, B.G. & Carr, B.R. (2018). The Normal Menstrual Cycle and the Control of Ovulation. Endotext. NCBI Bookshelf. View source
- Fehring, R.J., Schneider, M. & Raviele, K. (2006). Variability in the phases of the menstrual cycle. Journal of Obstetric, Gynecologic & Neonatal Nursing, 35(3), pp.376–384. doi:10.1111/j.1552-6909.2006.00051.x
- Lenton, E.A., Landgren, B.M. & Sexton, L. (1984). Normal variation in the length of the follicular phase of the menstrual cycle: effect of chronological age. British Journal of Obstetrics and Gynaecology, 91(7), pp.681–684. doi:10.1111/j.1471-0528.1984.tb04830.x
- Wirth, M.M. et al. (2011). The effect of cortisol on emotional responses. Hormones and Behavior, 59(5), pp.603–611.
- Macklon, N.S. & Fauser, B.C. (2001). Follicle-stimulating hormone and advanced follicle development in the human. Archives of Medical Research, 32(6), pp.595–600.
- Amin, Z., Canli, T. & Epperson, C.N. (2005). Effect of estrogen-serotonin interactions on mood and cognition. Behavioral and Cognitive Neuroscience Reviews, 4(1), pp.43–58. doi:10.1177/1534582305277152
- Roney, J.R. & Simmons, Z.L. (2013). Hormonal predictors of sexual motivation in natural menstrual cycles. Hormones and Behavior, 63(4), pp.636–645.
- Bigelow, J.L. et al. (2004). Mucus observations in the fertile window: a better predictor of conception than timing of intercourse. Human Reproduction, 19(4), pp.889–892. doi:10.1093/humrep/deh173
- Schmalenberger, K.M. et al. (2025). Menstrual Cycle Phase Influences Cognitive Performance in Women. Biology, 14(8), 1060.
- Mansour, D. et al. (2025). Cyclical fluctuations of iron biomarkers in women: Diagnostic implications for iron deficiency. Blood Advances.
- Higdon, J.V. et al. (2007). Cruciferous vegetables and human cancer risk. Nutrition Reviews, 65(12), pp.S68–S73.
- Karayiannis, D. et al. (2018). Adherence to the Mediterranean diet and IVF success rate among non-obese women attempting fertility. Human Reproduction, 33(3), pp.494–502. doi:10.1093/humrep/dey003
- McNulty, K.L. et al. (2020). The Effects of Menstrual Cycle Phase on Exercise Performance in Eumenorrheic Women: A Systematic Review and Meta-Analysis. Sports Medicine, 50(10), pp.1813–1827. doi:10.1007/s40279-020-01319-3
- Wilcox, A.J., Weinberg, C.R. & Baird, D.D. (1995). Timing of sexual intercourse in relation to ovulation. New England Journal of Medicine, 333(23), pp.1517–1521. doi:10.1056/NEJM199512073332301
Medical Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always consult your healthcare provider before making changes to your diet, exercise routine, or fertility plan. Every woman's cycle is different — what's described here represents general patterns, not a diagnosis.
All my Free Resources. No spam. Unsubscribe anytime.















