💡 Quick Answer
An AMH (anti-Müllerian hormone) blood test measures your ovarian reserve — the estimated number of eggs remaining. Normal AMH is roughly 1.0–3.5 ng/mL depending on age. It costs £30–£150 privately in the UK or $50–$200 in the US, and can be taken on any day of your cycle. AMH tells you about egg quantity, not quality — a low result doesn't mean you can't get pregnant.
Key Takeaways
- AMH measures ovarian reserve (egg quantity), not egg quality or your ability to conceive naturally
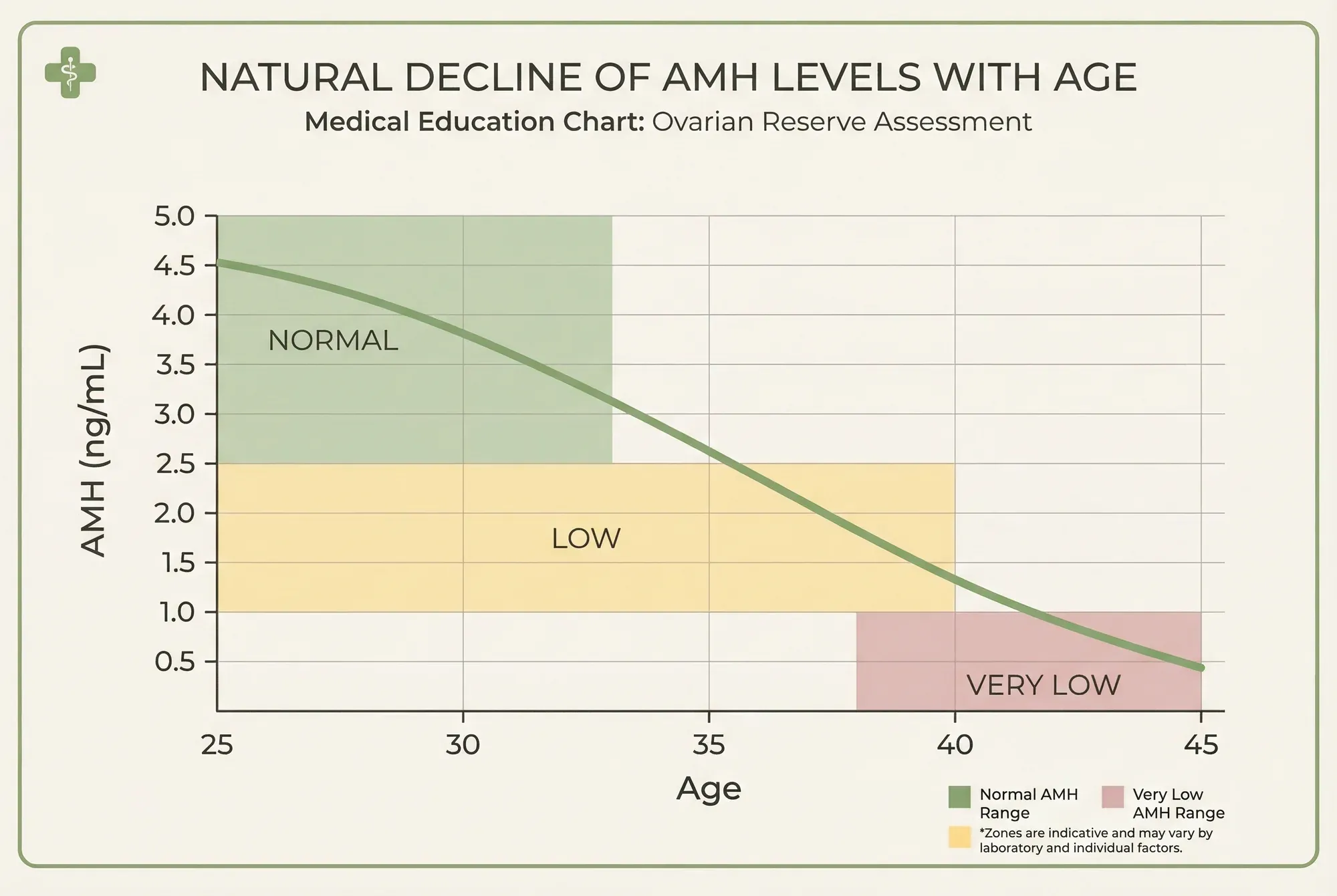
- Normal range varies by age: ~3.0+ ng/mL at 25, ~2.5 ng/mL at 30, ~1.5 ng/mL at 35, ~1.0 ng/mL at 40
- Unlike most fertility hormones, AMH can be tested on any day of your menstrual cycle
- NHS rarely covers AMH testing — private costs range from £30–£150 in the UK, $50–$200 in the US
- At-home AMH tests are clinically validated and can be a good starting point if clinic access is limited
- A low AMH result is not a diagnosis of infertility — women with low AMH conceive naturally every day
If you've spent any time reading about fertility, you've probably come across AMH. It's become the fertility test — the one number women fixate on, the one clinics order first, and the one that sends people spiralling at 2am when they Google what their results mean.
I understand why. When someone tells you a single blood test can estimate how many eggs you have left, it feels like a verdict on your future. But AMH is both more useful and more limited than most people realise, and understanding what it actually tells you (and what it doesn't) can save you a lot of unnecessary panic.
Here's everything you need to know — from what the test involves to what your numbers actually mean.
What Is an AMH Test?
AMH stands for anti-Müllerian hormone. It's a protein produced by the granulosa cells that surround your developing egg follicles — specifically the small antral follicles and pre-antral follicles in your ovaries.
The more developing follicles you have, the more AMH they produce. So your AMH blood test result gives an indirect estimate of your ovarian reserve — the pool of eggs available for future ovulation.
It's a simple blood draw. No fasting required. And unlike FSH or oestradiol (which fluctuate throughout your cycle), AMH levels remain relatively stable, which means you can take an AMH test on any day of your menstrual cycle. That's a genuine advantage — it makes scheduling much easier than other fertility blood tests.
The test is usually processed using one of two standardised assays: the Elecsys AMH Plus (Roche) or the Access AMH (Beckman Coulter). Results come back in 1–5 days depending on the lab, reported in either ng/mL or pmol/L. To convert: 1 ng/mL = 7.14 pmol/L.
What Does AMH Actually Tell You?
AMH tells you approximately how many eggs you have remaining relative to what's expected for your age. That's it. And that distinction matters enormously.
AMH does NOT tell you:
- Egg quality — a woman with low AMH can have perfectly healthy eggs
- Whether you can get pregnant naturally — a landmark 2017 study by Steiner et al. in JAMA followed 750 women aged 30–44 and found that women with low AMH had the same chance of conceiving naturally as women with normal AMH
- When you'll reach menopause — AMH correlates with egg supply but can't predict your exact timeline
- Your overall fertility — fertility depends on egg quality, fallopian tube function, uterine health, partner factors, and dozens of other variables
What AMH IS useful for:
- IVF planning — AMH predicts how many eggs you're likely to retrieve during a stimulation cycle. This is where it's genuinely most valuable.
- PCOS diagnosis support — very high AMH (above 5.0 ng/mL) can support a PCOS diagnosis, since polycystic ovaries contain many small follicles
- Baseline tracking — knowing your AMH at 28 gives you a reference point to compare at 33
- Informed decision-making — if your AMH is declining faster than expected, you might choose to pursue egg freezing or adjust your family planning timeline
I always tell clients this: AMH is a piece of the puzzle, not the whole picture. It's the most commonly misunderstood fertility test because the number feels so definitive when it's actually just one data point.
AMH Levels by Age: What's Normal?
AMH naturally declines with age as your egg supply diminishes. Here are approximate normal ranges based on published reference data:
| Age | Average AMH (ng/mL) | Low AMH Threshold | What It Means |
|---|---|---|---|
| Under 25 | 3.0–5.0 | Below 2.0 | Peak ovarian reserve; high egg count expected |
| 25–30 | 2.5–4.0 | Below 1.5 | Healthy reserve; good response expected to IVF stimulation |
| 30–35 | 1.5–3.5 | Below 1.0 | Gradual natural decline; still within normal fertility range |
| 35–38 | 1.0–2.5 | Below 0.7 | Noticeable decline; IVF may require adjusted protocols |
| 38–40 | 0.7–1.5 | Below 0.5 | Reduced reserve; time-sensitive decisions may be relevant |
| 40–42 | 0.3–1.0 | Below 0.3 | Low reserve typical for age; IVF yields may be lower |
| Over 43 | 0.1–0.5 | Below 0.1 | Very low reserve; approaching perimenopause |
Important context: These ranges are guidelines, not absolutes. Individual variation is enormous. A 35-year-old with an AMH of 0.8 ng/mL has lower-than-average reserve but could absolutely conceive naturally. A 28-year-old with an AMH of 5.5 ng/mL might warrant PCOS investigation. The number only makes sense in the context of your age, symptoms, and overall health picture.
Also note: reference ranges differ between labs and assays. Always compare your result to the reference range printed on YOUR lab report, not a generic chart from the internet. If your result is in pmol/L, divide by 7.14 to get the ng/mL equivalent.
When to Take an AMH Test
One of the most common questions I get asked is when to take AMH test. The short answer: whenever works for you. You can take an AMH blood test on any day of your menstrual cycle — that's one of its key advantages over other fertility tests like FSH or oestradiol, which need to be drawn on days 2–5.
Consider getting an AMH test if:
- You're over 30 and planning to delay pregnancy by several years
- You're considering egg freezing and want to estimate likely yield
- You're starting IVF and your clinic needs it for protocol planning
- You have a family history of early menopause
- You've been diagnosed with or suspected of having PCOS
- You've had ovarian surgery or chemotherapy (both can reduce reserve)
- You simply want a baseline for future comparison
When NOT to rely on AMH alone:
- If you're taking hormonal contraception — the pill, patch, ring, and hormonal IUDs can suppress AMH levels by 20–30%, giving a falsely low reading. Most clinicians recommend testing at least 3 months after stopping hormonal contraception.
- If you're under 25 and not planning pregnancy for years — AMH at this age is interesting information but rarely changes decisions
- If you're looking for a "fertility score" — AMH isn't that, and treating it as one leads to unnecessary anxiety
AMH Test Cost: UK and US Pricing
One of the most common questions I hear: how much does an AMH test actually cost? The answer depends heavily on where you live and how you access it.
UK Pricing
The NHS rarely covers AMH testing unless you're already referred to a fertility clinic and meet specific criteria (typically under 43, trying for 12+ months, or 6+ months if over 36). If you're testing proactively or "just to know," you'll need to go private.
- NHS fertility clinic: Free if referred, but wait times can be 3–6 months
- Private via NHS lab (e.g., Gloucestershire Hospitals NHS): From £30 — this is genuinely the cheapest option if available in your area
- Private fertility clinic: £80–£150 (London Pregnancy Clinic: £80, Medical Express Clinic: £149)
- At-home test kit (e.g., Hertility, Mira): £99–£149 including interpretation
US Pricing
- Fertility clinic with insurance: Often covered if part of an infertility workup, but you typically need to prove 12 months of unsuccessful trying first
- Out-of-pocket at clinic or lab: $50–$200 depending on location
- TLC Fertility (remote + Labcorp draw): $99 including consultation
- At-home test (Modern Fertility / Ro): ~$159 for multi-hormone panel including AMH
- LetsGetChecked: ~$139 for ovarian reserve test
Price alone shouldn't drive your decision. The cheapest test gives you a number. A test through a clinic gives you a number plus a professional who can explain what it means for YOUR situation — and that context matters enormously with AMH.
At-Home AMH Tests: Are They Accurate?
The at home AMH test market has grown significantly in the last few years, and at-home AMH tests have become increasingly popular, and the good news is they're genuinely clinically validated. A 2022 study found that finger-prick AMH testing was "non-inferior" to standard venous blood draws — meaning the results were clinically equivalent.

The main at-home options:
- Modern Fertility (now part of Ro): Finger-prick test, results in about 10 days. Tests AMH plus up to 7 other hormones. US-based, CLIA-certified labs. ~$159.
- LetsGetChecked: Finger-prick collection returned by post, results reviewed by a doctor. CLIA-approved labs. ~$139 for ovarian reserve panel.
- Hertility (UK): Finger-prick test, NHS-accredited labs, includes gynaecologist review. £99–£149. Particularly popular in the UK.
- Mira: Urine-based hormonal tracking (not blood AMH). Different technology — tracks LH, oestrogen, PdG, and FSH rather than AMH directly.
The limitations of at-home tests:
- Finger-prick samples are smaller, which can occasionally affect accuracy at very low AMH levels
- You get a number and an explanation, but not the clinical context of sitting with a specialist
- If your result is low, you'll likely need a follow-up with a fertility specialist anyway
My take: at-home AMH tests are a reasonable starting point, especially if clinic access is limited or you want a baseline before committing to a full fertility workup. But if your result comes back low or unexpectedly high, book a consultation with a reproductive endocrinologist for proper interpretation.
Understanding Your AMH Blood Test Results
You've got your number. Now what?

High AMH (Above 3.5 ng/mL or 25 pmol/L)
If you're researching your AMH test fertility implications, this section breaks down exactly what each range means. A high AMH usually means you have a larger-than-average ovarian reserve for your age. In the context of IVF, this is generally positive — it suggests a good response to stimulation and a higher egg retrieval count.
However, very high AMH (above 5.0 ng/mL) can indicate polycystic ovary syndrome (PCOS). In PCOS, the ovaries contain many small follicles that collectively produce excess AMH. If your AMH is significantly above the expected range for your age and you have other symptoms (irregular periods, acne, excess hair growth), discuss PCOS screening with your doctor.
High AMH also correlates with a higher risk of ovarian hyperstimulation syndrome (OHSS) during IVF — something your fertility specialist should account for in your stimulation protocol.
Normal AMH (1.0–3.5 ng/mL or 7–25 pmol/L)
This is the range most women fall into if they're within a few years of the average for their age. A "normal" AMH means your ovarian reserve appears typical. For IVF, it suggests a standard stimulation protocol should work well.
Don't get too attached to where you fall within "normal." An AMH of 1.2 at age 32 and an AMH of 3.2 at age 32 are both normal — but they tell different stories about the pace of your ovarian ageing. Context matters.
Low AMH (Below 1.0 ng/mL or 7 pmol/L)
This is the result that terrifies people, and I want to be really clear about something: low AMH does not mean you can't get pregnant.
The 2017 Steiner et al. study in JAMA is worth repeating here. They followed 750 women aged 30–44 who were trying to conceive naturally. Women with low AMH (below 0.7 ng/mL) had the same probability of conceiving within 12 months as women with normal AMH. The 12-cycle cumulative pregnancy rate was 65% for low AMH versus 62% for normal AMH. No significant difference.
What low AMH DOES mean:
- You have fewer eggs remaining than average for your age
- In IVF, you may retrieve fewer eggs per cycle (requiring potentially more cycles)
- Your window for fertility preservation (egg freezing) may be narrower
- It's worth investigating sooner rather than waiting if you're planning to conceive
What low AMH does NOT mean:
- Your eggs are bad quality
- You're infertile
- You need IVF to conceive
- You should panic
Very Low AMH (Below 0.3 ng/mL or 2 pmol/L)
At this level, ovarian reserve is significantly depleted. Natural conception is still possible but less likely, and IVF outcomes may be more challenging. If you're in this range and wanting to conceive, see a reproductive endocrinologist promptly — timing matters more when reserve is very low.
Some clinics use "undetectable" AMH as a threshold below which they won't proceed with IVF using your own eggs. If you receive this result, seek a second opinion — protocols and thresholds vary between clinics, and some specialists have experience optimising outcomes for very low reserve.
Factors That Affect Your AMH Level
Your AMH isn't a fixed number. Several factors can influence it:
- Age: The biggest factor. AMH declines naturally from your mid-20s onward, with acceleration after 35.
- Hormonal contraception: The combined pill, patch, and ring can suppress AMH by 20–30%. Test at least 3 months after stopping for an accurate baseline.
- Vitamin D: Low vitamin D is associated with lower AMH levels. A 2018 study by Dennis et al. found that vitamin D supplementation increased AMH in vitamin D-deficient women.
- Smoking: Active smoking lowers AMH. Quitting may partially reverse this effect.
- BMI: Obesity is associated with lower AMH, while PCOS-related high BMI can paradoxically show high AMH due to the condition itself.
- Ovarian surgery: Any surgery on the ovaries (cyst removal, endometriosis excision) can reduce AMH.
- Chemotherapy/radiation: Can significantly reduce ovarian reserve. Fertility preservation should be discussed before treatment.
- DHEA and CoQ10: Some evidence suggests these supplements may support ovarian function, though the research on directly raising AMH is limited.
AMH Testing and IVF: Why It Matters Most Here
If there's one context where AMH genuinely earns its reputation, it's IVF planning.
Your AMH level helps your fertility specialist choose the right stimulation protocol. Higher AMH means your ovaries are likely to respond strongly to gonadotropin medications — so they'll use lower doses to avoid OHSS. Lower AMH means they may need higher doses or different protocols (like mini-IVF or natural cycle IVF) to maximise your chances.
Research by La Marca et al. (2010) in Human Reproduction Update established AMH as the single best predictor of ovarian response to stimulation — outperforming age, FSH, and antral follicle count (AFC) for predicting how many eggs will be retrieved.
Typical IVF response predictions based on AMH:
- AMH above 3.5 ng/mL: High response likely (15+ eggs). Lower stimulation dose recommended. Higher OHSS risk.
- AMH 1.0–3.5 ng/mL: Normal response (8–15 eggs). Standard protocols.
- AMH 0.5–1.0 ng/mL: Reduced response (3–8 eggs). May need adjusted protocols.
- AMH below 0.5 ng/mL: Poor response likely (1–3 eggs). Mini-IVF or accumulation cycles may be considered.
But even here, AMH isn't destiny. Some women with low AMH respond better than expected. Some with high AMH respond poorly. It's a prediction tool, not a guarantee.
Common AMH Myths That Cause Unnecessary Panic
I've sat across from clients who came in convinced their fertility was over because of an AMH result. In almost every case, the panic was based on misconceptions. Let me address the biggest ones.
"My AMH dropped since last year — my fertility is crashing"
AMH naturally declines with age. A drop from 2.8 to 2.3 ng/mL over a year is completely expected and not a crisis. AMH also has natural fluctuations — it can vary by 10–20% between tests taken on different days, depending on your cycle, lab assay, and even seasonal variation. One study found AMH levels were slightly higher in spring and summer. Only a significant, sustained decline warrants concern.
"My AMH is low so I need to freeze my eggs immediately"
Low AMH means fewer eggs will be available, but "fewer" doesn't mean "none." The urgency depends on how low, your age, and your timeline. If you're 31 with an AMH of 0.9, you have time to plan. If you're 39 with an AMH of 0.3, the window is genuinely narrower. Either way, the decision deserves a conversation with a specialist — not a panic reaction.
"My friend's AMH is higher than mine — she's more fertile"
AMH isn't a competition. Two women the same age with AMH values of 1.5 and 3.5 could have identical chances of natural conception. The woman with 3.5 has more eggs in reserve, but fertility depends on dozens of factors beyond egg count. Comparing AMH numbers between individuals is meaningless without full clinical context.
"I can boost my AMH with supplements"
Some supplements (DHEA, CoQ10, vitamin D) may support ovarian function, and vitamin D supplementation has been shown to raise AMH in deficient women. But you can't meaningfully "boost" your ovarian reserve through supplements — AMH reflects how many follicles you have, and that number is fundamentally determined by biology and age. What you CAN do is support the quality of the eggs you have through nutrition, lifestyle, and targeted supplementation.
"My GP said my AMH is fine so I don't need to worry"
GPs are brilliant at many things, but fertility hormone interpretation isn't always their speciality. "Fine" from a GP might mean "within the lab reference range" — but reference ranges are wide and don't account for your age or reproductive goals. If you have specific fertility concerns, see a reproductive endocrinologist who interprets these results daily.
The Bottom Line
AMH is the most useful single fertility blood test we have — and it's also the most misunderstood. It tells you about egg quantity, not quality. It predicts IVF response, not natural conception chances. And a low number, while worth taking seriously, is not a diagnosis of infertility.
If you're thinking about getting tested, do it. Knowledge is better than anxiety, and a baseline AMH at 30 is genuinely useful information for future planning. Just promise me you won't read the result at midnight and spiral. Take the number to a professional who can put it in context — because context is everything with this test.
And if your result wasn't what you hoped for: take a breath. The research is clear that low AMH doesn't prevent natural conception. It changes the timeline and may influence which paths you explore — but it doesn't close the door.
Frequently Asked Questions
How much does an AMH test cost?
In the UK, AMH test cost ranges from £30 (NHS labs offering private access) to £150 (London private clinics). At-home kits like Hertility cost £99–£149. In the US, the AMH test price ranges from $50 to $200 out-of-pocket at clinics, or ~$139–$159 for at-home options like Modern Fertility or LetsGetChecked. The NHS covers it free if you're referred to a fertility clinic, but proactive testing requires private payment.
Can you take an AMH test at home?
Yes. At-home AMH tests use a finger-prick blood sample mailed to a certified lab. A 2022 study confirmed that finger-prick AMH testing produces clinically equivalent results to standard blood draws. Leading at-home options include Modern Fertility (US, ~$159), LetsGetChecked (US/UK, ~$139), and Hertility (UK, £99–£149). If your result is abnormal, follow up with a fertility specialist for proper interpretation.
When should I take an AMH test?
AMH can be tested on any day of your menstrual cycle — unlike FSH or oestradiol, which must be drawn on days 2–5. However, avoid testing while on hormonal contraception (the pill can suppress AMH by 20–30%). Wait at least 3 months after stopping for an accurate result. Consider testing if you're over 30 and planning to delay pregnancy, considering egg freezing, starting IVF, or have a family history of early menopause.
What is a good AMH level to get pregnant?
For natural conception, AMH level matters less than most people think. The 2017 JAMA study found that women with low AMH (below 0.7 ng/mL) had the same chance of conceiving naturally as women with normal AMH. For IVF, an AMH of 1.0–3.5 ng/mL typically predicts a good response. But "good AMH" is always relative to your age — an AMH of 1.5 ng/mL is reassuring at 38 but would warrant investigation at 28.
Does low AMH mean I'm infertile?
No. Low AMH means you have fewer eggs remaining than average for your age, but it says nothing about egg quality or your ability to conceive. Many women with low AMH get pregnant naturally without assistance. Where low AMH matters most is IVF (fewer eggs retrieved per cycle) and timing (a narrower window for fertility preservation). A low result is worth discussing with a specialist, but it is not a diagnosis of infertility.
What do AMH blood test results mean?
AMH blood test results estimate your ovarian reserve. Results above 3.5 ng/mL suggest high reserve (or possible PCOS if very high). Between 1.0–3.5 ng/mL is considered normal for most reproductive ages. Below 1.0 ng/mL indicates reduced reserve. Below 0.3 ng/mL suggests significantly depleted reserve. Always interpret your result in the context of your age and the reference range on your specific lab report, as assay methods and units (ng/mL vs pmol/L) vary between laboratories.
References
- Steiner AZ, et al. Association between biomarkers of ovarian reserve and infertility among older women of reproductive age. JAMA. 2017;318(14):1367-1376. doi:10.1001/jama.2017.14588
- La Marca A, et al. Anti-Müllerian hormone (AMH) as a predictive marker in assisted reproductive technology (ART). Hum Reprod Update. 2010;16(2):113-130.
- Dennis NA, et al. The level of serum anti-Müllerian hormone correlates with vitamin D status in men and women but not in boys. J Clin Endocrinol Metab. 2012;97(7):2450-2455.
- Cleveland Clinic. Anti-Mullerian Hormone (AMH) Test: Purpose, Levels & Results. 2022. clevelandclinic.org
- MedlinePlus. Anti-Müllerian Hormone Test. National Library of Medicine. medlineplus.gov
- Dewailly D, et al. The physiology and clinical utility of anti-Müllerian hormone in women. Hum Reprod Update. 2014;20(3):370-385.
- Bonifacio M, Bradley CK, Karia S, et al. The original Beckman Coulter Generation II assay significantly underestimates AMH levels compared with the revised protocol. J Assist Reprod Genet. 2015;32(11):1691-1696.
Medical Disclaimer: This article is for informational purposes only and does not constitute medical advice. AMH results should always be interpreted by a qualified healthcare provider in the context of your individual circumstances. Always consult your doctor or a reproductive endocrinologist before making decisions based on fertility test results.
All my Free Resources. No spam. Unsubscribe anytime.